What Causes Receding Gums in Adults? Symptoms & Cures
What causes receding gums in adults? Our Fair Lawn dentists explain the causes & treatments to restore your smile. Schedule a consultation today.
What causes receding gums in adults? Our Fair Lawn dentists explain the causes & treatments to restore your smile. Schedule a consultation today.

If you’ve looked in the mirror and thought your teeth seem longer, or you’ve started feeling a sharp sting when you drink something cold, you’re not overreacting. Those are common ways adults first notice gum recession. It often starts subtly, then becomes harder to ignore once the tooth root is exposed and everyday things like brushing or eating feel uncomfortable.
A lot of patients searching for what causes receding gums in adults are trying to answer two questions at once. First, “Is this really happening to me?” Second, “Can anything be done before it gets worse?” The answer to both is yes. Gum recession is common, it has identifiable causes, and the right dental care can help stop further damage and protect your smile.
For adults in Fair Lawn, Ridgewood, and Glen Rock, this concern often shows up during a routine cleaning and exam, a cosmetic consultation, or even a visit for tooth sensitivity. Sometimes it’s linked to gum disease. Sometimes it’s related to brushing habits, teeth grinding, smoking, bite problems, or inherited thin gum tissue. Often, it’s a combination.
Gum recession means the gum tissue has pulled back from the tooth, exposing more of the tooth surface or even the root. Because this usually happens gradually, many adults don’t notice it right away. They just sense that something looks different, or they start avoiding cold drinks on one side of the mouth.
The most important thing to know early is this: periodontal disease is the primary cause of receding gums in adults, affecting 42% of U.S. adults aged 30 and older, according to the National Institute of Dental and Craniofacial Research data on periodontal disease in adults. That’s why visible gum changes should never be brushed off as “just getting older.”

Some signs are visual. Others are more about sensation.
People often get confused here because gum recession doesn’t always hurt. You can have ongoing tissue loss without dramatic pain. That’s one reason many adults discover it during a dental exam rather than at home.
Practical rule: If your teeth look longer, feel more sensitive, or your gums seem to be pulling away in one area, it’s worth having it checked before the problem becomes deeper and harder to treat.
A simple way to think about it is that early recession affects comfort and appearance. More advanced recession starts affecting stability and long-term tooth health.
| Stage | What you may notice | Why it matters |
|---|---|---|
| Early | Mild sensitivity, slight uneven gumline, teeth look a bit longer | The cause may still be easier to control |
| Moderate | More visible root exposure, tenderness when brushing, recurring inflammation | The root is more vulnerable to wear and decay |
| Advanced | Deep spaces near teeth, shifting appearance, increasing discomfort | Support around the tooth may be compromised |
If you’ve also noticed bleeding when brushing, bad breath, or puffiness in the gums, there may be inflammation involved too. For a closer look at related warning signs, this guide on signs of gum disease can help connect the dots.
A gum recession exam shouldn’t feel mysterious or intimidating. Most adults are relieved once they understand what the dentist is looking for.
The exam usually includes:
The underlying causes of gum recession are critical, as two individuals can present with visually similar conditions. One may have inflammation from periodontal disease. Another may have mechanical wear from brushing too hard or clenching at night. The treatment plan changes depending on the cause.
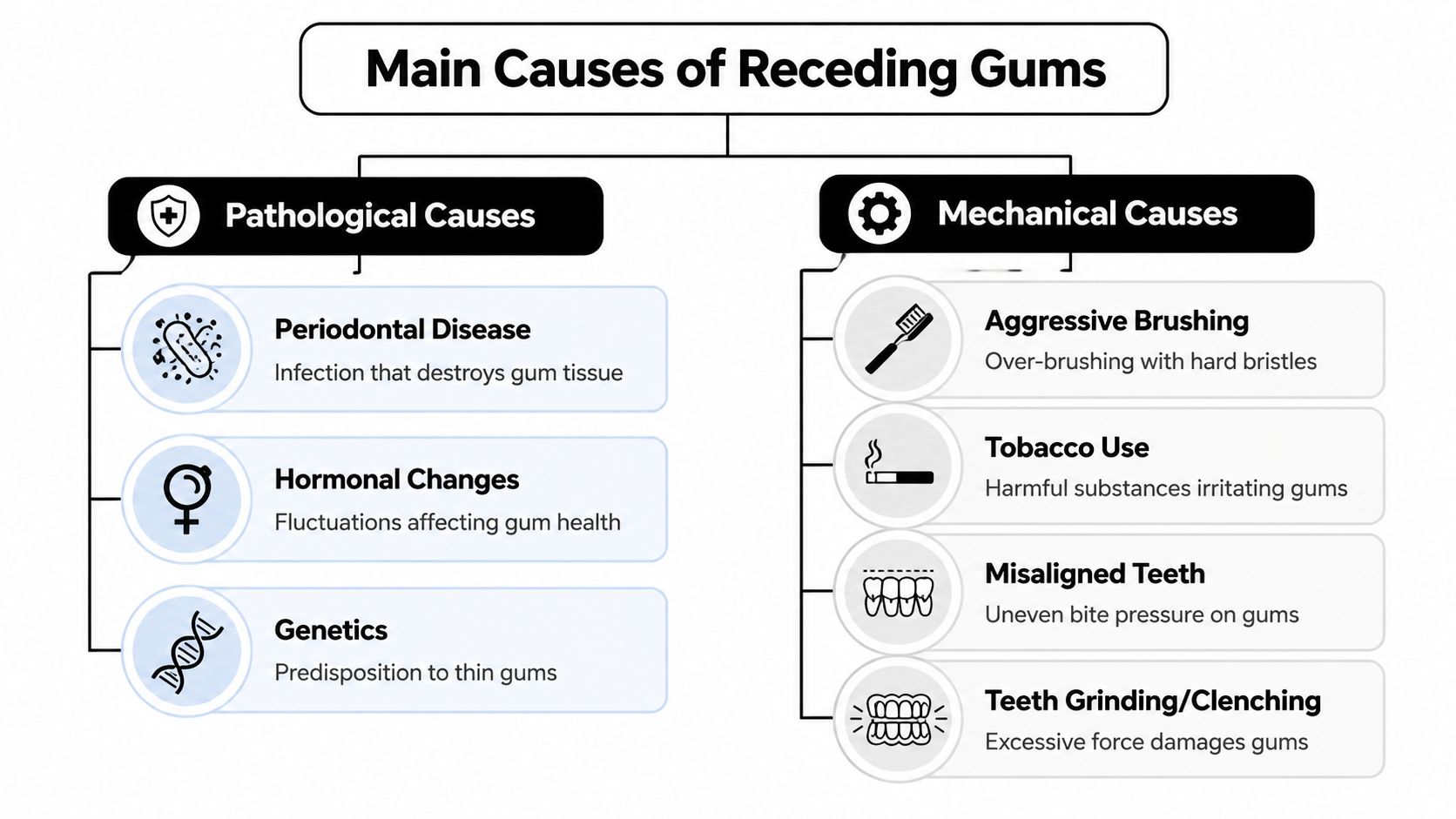
When adults ask what causes receding gums, they often expect a single answer. In reality, recession usually develops through either pathological causes or mechanical causes, and sometimes both are present at the same time. That’s why one person needs deep periodontal treatment while another needs changes in brushing technique, bite correction, or a nightguard.
This is the main medical cause in adults. Plaque bacteria collect around the gumline. If that buildup isn’t thoroughly removed, the tissue becomes inflamed. Over time, the infection can move deeper and start affecting the structures that support the tooth.
The tissue damage isn’t just surface irritation. Periodontal disease operates through an inflammatory cascade where bacterial infection triggers enzymes that digest connective tissue and bone, as described in this explanation of gum recession causes and progression. That same source notes that nearly 88% of adults over 65 have at least one site of gum recession.
Here’s where many patients get tripped up: they assume recession means the gum “shrinks.” In periodontal disease, the process is more destructive than that. The supporting attachment around the tooth breaks down, the bone level can drop, and the gum margin moves lower as a result. That’s why untreated gum disease can affect both appearance and tooth stability.
Some recession starts from repeated physical trauma instead of infection. A common example is brushing too hard with a stiff hand motion, especially along the outer gumline of the canines and premolars.
This can happen even to people who are very committed to oral hygiene. In fact, it often happens to people who are trying to do the right thing but are using too much force. The gum tissue near the tooth is delicate. If you scrub instead of clean, the tissue can wear away little by little.
A few clues point toward this kind of cause:
A soft-bristled brush, lighter pressure, and better technique can make a big difference when mechanical trauma is the issue.
Recession doesn’t always mean poor hygiene. Sometimes it means the technique has been too forceful for too long.
Grinding and clenching create a different kind of stress. Instead of wearing the gum from the outside, they place excess force on the teeth and the ligament system that supports them.
That force can irritate the tissues around the teeth, especially if the bite is uneven. Some adults notice this pattern when they wake with jaw tension, headaches, flattened teeth, or soreness near one side of the mouth. Others don’t realize they grind until the dentist spots the wear.
Bruxism doesn’t cause every case of recession, but it can make a vulnerable area worse. If a tooth is already under inflammatory stress or has thin gum tissue, heavy bite pressure can accelerate the problem.
Crooked teeth aren’t only a cosmetic issue. In some adults, misalignment changes where force lands when they bite and chew. If one tooth sits too far forward or outside the natural arch, the gum and bone around that tooth may be thinner and less protected.
That’s one reason recession often appears around certain lower front teeth or prominent canines. The tooth position itself can create a weak point.
This matters for treatment because a person may improve brushing and still keep losing gum tissue if the bite remains unbalanced. In some cases, orthodontic treatment such as Invisalign or Six Month Smiles may be part of the bigger solution. That’s not just about appearance. It can also support healthier force distribution and improve access for cleaning.
Smoking affects the gums in more than one way. It can irritate oral tissues, support bacterial buildup, and make gum disease harder to control. It also complicates healing. If recession has both inflammatory and mechanical causes, tobacco use often makes the whole situation harder to stabilize.
This is one reason adults with gum recession sometimes need a broader plan that includes periodontal treatment, habit changes, and long-term maintenance.
Two patients can walk in with exposed roots and sensitivity, but their care may look very different.
| Primary cause | Main problem | Common treatment direction |
|---|---|---|
| Periodontal disease | Infection and attachment loss | Deep cleaning, periodontal therapy, maintenance |
| Aggressive brushing | Repeated surface trauma | Technique correction, gentler tools, desensitizing care |
| Grinding or clenching | Pressure overload | Bite evaluation, nightguard, wear protection |
| Misalignment | Uneven force and hard-to-clean areas | Orthodontic planning, cleaning support |
| Combined causes | Infection plus trauma or pressure | Layered treatment using restorative dentistry or cosmetic dentistry when needed |
That’s why guessing at the cause from a mirror alone can be misleading. Root coverage, cosmetic dentistry, and restorative dentistry can improve comfort and appearance, but lasting results depend on identifying what started the recession in the first place.
Some adults do everything “right” and still develop gum problems. That can feel frustrating until you understand that gum health isn’t determined by brushing alone. Your inherited tissue type, your medical history, and your daily habits all shape how your gums respond over time.

Some people naturally have thinner gum tissue or a stronger family history of advanced gum disease. That doesn’t guarantee recession, but it does mean the tissues may be less forgiving when plaque, bite pressure, or inflammation are present.
Many people don't realize that genetics can account for up to 50% of the variance in severe periodontitis cases, according to this discussion of genetic predisposition and gum recession. In practical terms, that means two adults with similar oral hygiene habits may not have the same outcome.
If your parents or siblings have had loose teeth, gum grafting, advanced periodontal treatment, or early tooth loss, that history matters. It’s worth mentioning during a dental exam because it changes how closely your gums should be monitored.
Lifestyle and health conditions can make vulnerable gums more likely to break down.
Smoking is a major example. It promotes plaque retention, irritates the tissues, and makes healing less predictable. Diabetes also matters because high blood sugar can affect inflammation and the body’s response to infection. Nutrition plays a role as well. Vitamin C supports collagen health, so deficiency may weaken gum attachment and repair.
Here's a simple way to understand it:
Family history is not a verdict. It’s a reason to monitor your gums earlier and more carefully.
Many generic online articles often fall short on this point. They list causes, but they don’t explain why one adult gets localized recession while another develops broader periodontal breakdown. The answer often lies in how several factors overlap.
A patient might have thin inherited gum tissue, mild crowding, and nighttime clenching. Another might have controlled brushing habits but struggle with smoking and diabetes. Those aren’t the same clinical picture, so they shouldn’t get the same advice.
A thoughtful dental exam looks at the pattern, not just the symptom. That’s especially helpful if you’ve been told to “brush softer” but the recession keeps progressing anyway.
Once gums recede, the next question is usually whether they can be fixed. The answer depends on how much tissue has been lost, what caused it, and whether the supporting structures around the teeth are healthy enough to stabilize first.
Some treatments focus on stopping the disease process. Others focus on covering exposed roots, reducing sensitivity, improving appearance, or correcting the bite conditions that helped create the problem.

If gum recession is tied to active periodontal disease, the first job is controlling infection below the gumline. That usually means scaling and root planing, often described as a deep cleaning. This removes plaque and tartar from areas a regular cleaning can’t reach and smooths the root surface so the tissue has a better chance to heal.
For many adults, this is the turning point. Bleeding decreases, inflammation calms down, and the tissue becomes easier to maintain. If you want a better sense of what that process involves, this overview of periodontal disease treatment explains the basics clearly.
When roots are exposed and the area is stable, a graft may be recommended. Gum grafting places tissue over the exposed root to improve protection, reduce sensitivity, and create a more natural gumline.
This can be especially helpful when recession affects visible front teeth or when the exposed root is at risk for wear and decay. In cosmetic cases, patients often care about symmetry. In functional cases, they care more about comfort while brushing and eating. Often, both goals matter.
A related option in selected cases is the Pinhole Surgical Technique, which repositions gum tissue through a very small entry point rather than a more traditional grafting approach. That can be appealing for adults who want a less invasive method when they’re good candidates.
Some recession won’t stay stable unless the mechanical cause is addressed. That’s where treatment gets more extensive.
Mechanical forces like teeth grinding can cause significant gum recession by overstressing the periodontal ligament cells, and smokers are up to six times more likely to develop gum recession than non-smokers, as described in this review of receding gum causes and treatment factors. In practice, that means treating the exposed root without treating the pressure can lead to disappointing results.
A nightguard may help if clenching or grinding is part of the pattern. If a tooth sits out of position and receives too much force, orthodontic treatment may help move it into a healthier position. For adults already interested in straighter teeth, that can make Invisalign or Six Month Smiles part of both a cosmetic and periodontal plan.
In severe cases, gum disease can lead to tooth mobility or tooth loss. If that happens, treatment may shift toward restorative dentistry. Depending on the situation, options may include crowns, bridges, dentures, or dental implants.
Implants aren’t the first topic in a recession exam, but they become relevant when a tooth can’t be saved or has already been lost. In those cases, the health of the surrounding gum and bone still matters. A stable periodontal foundation is what makes any long-term restoration more predictable.
Not every patient needs surgery. Not every patient needs orthodontics. The right plan comes from matching the treatment to the cause and the stage of the damage.
| Treatment | Best suited for | Main goal |
|---|---|---|
| Scaling and root planing | Recession with periodontal infection | Stop disease activity and reduce inflammation |
| Gum grafting | Exposed roots and lost tissue | Cover roots and improve protection |
| Pinhole Surgical Technique | Selected recession cases | Reposition tissue with a less invasive approach |
| Nightguard therapy | Grinding and clenching | Reduce pressure on teeth and gum support |
| Orthodontics | Misalignment and uneven force | Improve bite balance and cleanability |
| Dental implants or other restorative care | Teeth lost from advanced damage | Restore function and appearance |
The best recession treatment doesn’t just make the gumline look better. It removes the reason the tissue was failing in the first place.
Prevention starts with one simple idea: protect the gumline from both inflammation and trauma. That means your home routine matters, but so do regular professional cleanings and exams.

Many adults are surprised to learn that “brushing well” and “brushing hard” are not the same thing. Aggressive brushing is a leading mechanical cause of gum recession, and smoking puts people at over 60% risk for periodontal disease, according to the Cleveland Clinic overview of gum recession causes.
A good home routine usually includes:
If you’ve ever thought, “But I brush all the time, so why is this happening?” brushing force may be part of the answer.
Even a careful routine at home can’t fully manage tartar once it hardens below the gumline. That’s where dental cleaning, new patient exams, periodontal measurements, and dental x-rays become part of prevention instead of just diagnosis.
Regular visits help a dentist track small changes before they become large ones. A tiny shift in gum height, a deepening pocket, or a wear pattern from grinding is much easier to address early.
For a quick visual overview of better daily technique, this video can help reinforce what gentle, protective care should look like.
Small changes in technique can protect your gums more effectively than brushing harder ever will.
Starting with a new dentist is easier when you know what to expect. If you’re worried about gum recession, sensitivity, or changes in your smile, the first visit should feel calm, thorough, and focused on answers rather than pressure.
A new patient exam begins with listening. You may have noticed one sensitive tooth, a gumline that looks uneven in photos, or a spot that seems to keep getting worse. Those details matter because they help connect what you’re seeing at home with what the clinical exam reveals.
The evaluation goes beyond the visible gumline. The team looks at tooth position, bite forces, inflammation, previous dental work, root exposure, and the health of the surrounding bone. Digital imaging and modern diagnostic tools make that process more comfortable and more precise. If orthodontic factors are involved, tools such as iTero digital scanning can help assess tooth position without the mess of traditional impressions.
The bigger advantage is that the exam isn’t limited to teeth alone. A thorough exam at our practice goes beyond just your teeth. We consider systemic factors, as conditions like diabetes can double or triple periodontitis risk, and even Vitamin C deficiencies can impair gum health, as discussed in this article on systemic causes of gum recession and gum health. That broader view matters when recession is part of a larger oral health pattern.
Patients who feel nervous about treatment also have options. Sedation dentistry can help anxious adults complete needed care more comfortably. If the recession is tied to cosmetic concerns, the conversation can include gum reshaping, bonding, whitening, or other ways to restore confidence in your smile. If the issue is advanced and functional, the plan may involve periodontal therapy, restorative dentistry, or dental implants.
For families and adults in Fair Lawn, Ridgewood, and Glen Rock, convenience matters too. Flexible scheduling, a modern office, and financing options can make it easier to move forward with care instead of putting it off.
The first step is getting clear on the cause. Once you know why your gums are receding, the next step becomes much easier.
If you’re noticing sensitivity, exposed roots, or changes in your gumline, Dental Professionals of Fair Lawn can help you get answers and a personalized plan. Whether you need a new patient exam, periodontal care, cosmetic treatment, Invisalign, restorative dentistry, or guidance from an experienced dentist in Fair Lawn, NJ, the team is here to help you protect your smile with compassionate, advanced dental care. Schedule your consultation today.