What Are the Signs of Gum Disease? Spot Them Early.
What are the signs of gum disease - Learn what are the signs of gum disease: swollen gums, loose teeth, & more. Dental Professionals of Fair Lawn, NJ offers exp
What are the signs of gum disease - Learn what are the signs of gum disease: swollen gums, loose teeth, & more. Dental Professionals of Fair Lawn, NJ offers exp

You brush before work, rinse, and notice a little pink in the sink. Maybe your gums look puffy around one back tooth, or your breath still seems off by midday. Many patients ignore those changes because they are mild, intermittent, and often painless at first.
That is how gum disease often starts. Early signs can be reversible. Later signs can mean the infection has already moved beyond the gums and started affecting the bone and support around the teeth.
At Dental Professionals of Fair Lawn, we see that progression in patients from Fair Lawn, Ridgewood, and Glen Rock. The trade-off is usually straightforward. Coming in early often means a professional cleaning, better home care, and closer monitoring. Waiting can mean deeper treatment, more discomfort, higher cost, and in advanced cases, a risk to the teeth themselves.
To make this easier to judge, we have ranked the 8 most common signs from the earliest warning signs of gingivitis to the more urgent findings seen in periodontitis. That way, you can tell which changes are usually early and manageable, and which ones call for prompt dental care.
Some signs are subtle. Others should not be watched at home for long. If you are seeing bleeding, recession, looseness, pus, or changes in how your teeth come together, the order matters. So does timing.
Healthy gums usually look firm and fit closely around the teeth. When they become irritated, they often turn redder, look puffy, and feel sore when you brush or floss.
This is one of the earliest warning signs of gingivitis. In plain terms, the gums are inflamed because plaque has been sitting at the gumline long enough to trigger a reaction. At this stage, many patients assume they just brushed too hard or changed toothpaste. Sometimes that’s possible, but persistent swelling usually deserves a closer look.
You might notice that the gumline looks shiny instead of matte. The tissue may feel tender when you run floss between the teeth, or it may seem swollen around one back tooth where food tends to get trapped.
In the chair, this often shows up in two patterns:
For patients in Fair Lawn, this is the stage where simple changes can still make a big difference. Better brushing technique, better daily plaque removal, and a professional cleaning are often far more effective than switching from one over-the-counter rinse to another and hoping it settles down on its own.
Practical rule: If your gums have looked red or puffy for more than a short stretch, stop guessing and get them checked.
What tends to work:
What usually doesn’t work:
You finish brushing, rinse, and see pink in the sink again. If that keeps happening, treat it as an early warning sign, not a minor annoyance.
Bleeding during brushing or flossing often points to inflammation along the gumline. In this severity ranking, it still sits on the earlier, more reversible end of the spectrum. That is the good news. The trade-off is that people often ignore it because it does not hurt much, and that delay gives plaque and tartar more time to irritate the tissue.
Patients often tell me they stopped flossing because the area bled. I understand the instinct. In many cases, though, the tissue is bleeding because it is not being cleaned well enough between the teeth. Gentle daily flossing or another interdental cleaner usually helps calm inflamed gums over time, while avoiding the area tends to keep the cycle going.
Bleeding is also not perfectly reliable on its own. A patient can have early gum disease with frequent bleeding, while a smoker may have more advanced disease with less visible bleeding because blood flow in the gums is reduced. So I look at bleeding as one sign in a bigger pattern, not the whole diagnosis.
If one spot bleeds every time you brush or floss for several days, that deserves attention.
Our article on why gums bleed when you brush explains common causes and when an exam makes sense.
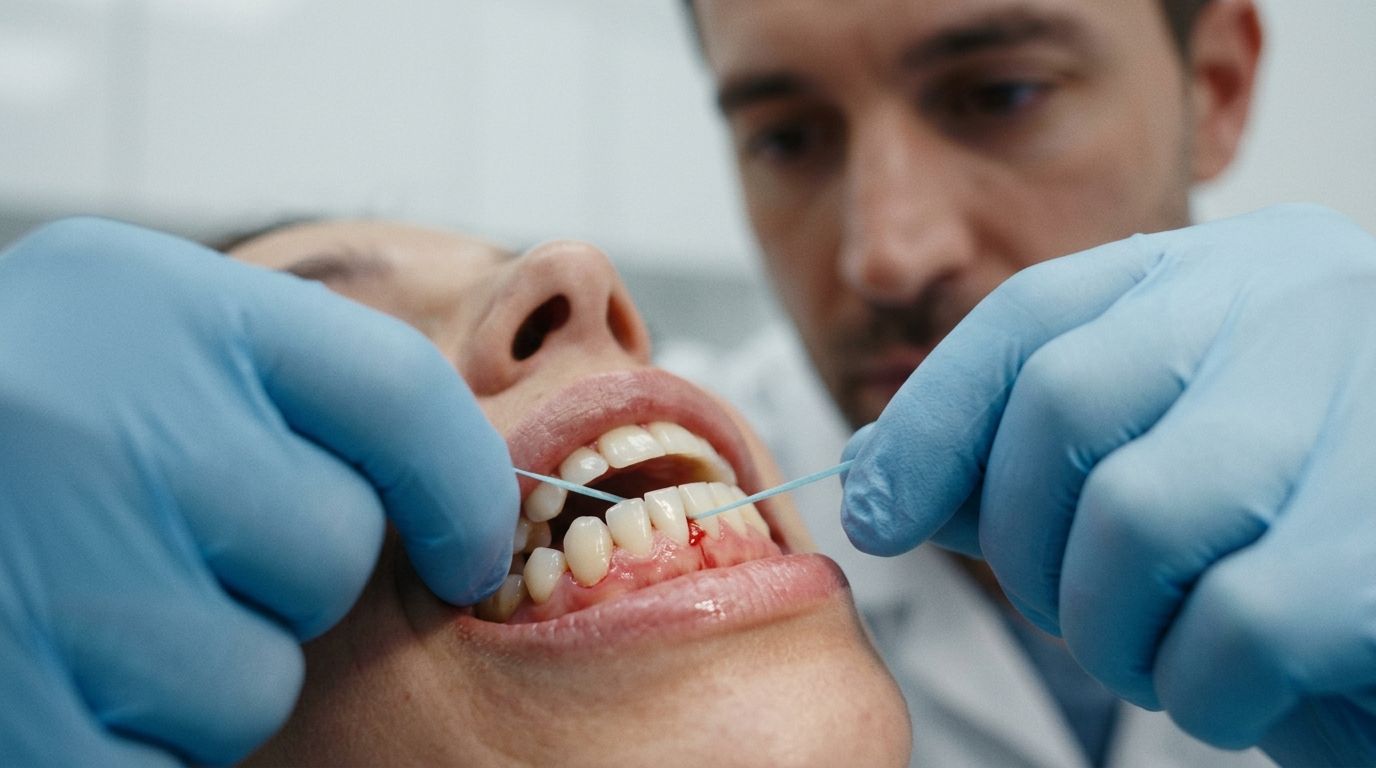
At this stage, home care still matters, but technique matters just as much.
Healthy gums should not bleed with normal brushing and flossing. Repeated bleeding is a reason to get checked.
A common early conversation goes like this. Someone in Fair Lawn says they brush twice a day, use mouthwash, keep mints in the car, and still feel unsure about their breath by lunchtime. That pattern deserves a closer look.
Persistent bad breath can be one of the stronger signs that gum inflammation is moving beyond simple surface irritation. Bacteria and debris collect along and below the gumline, and the odor tends to return quickly after brushing because the source is still there. In the severity ranking of gum disease signs, this usually sits above occasional redness or bleeding because it often suggests bacterial buildup that home care is not fully controlling.
Bad breath does not always mean gum disease. Dry mouth, sinus drainage, certain foods, medications, and cavities can all change breath odor. The trade-off is that people often spend weeks trying rinses, gum, or tongue scrapers before getting the gums checked, and that can delay treatment if periodontal infection is part of the problem.
What gets my attention is persistence. If the odor keeps coming back despite careful brushing, flossing, tongue cleaning, and hydration, the gums move higher on the list of likely causes. Family members often notice it first. Other patients tell us they feel dependent on mints all day.
Covering the smell rarely fixes the reason for it.
At Dental Professionals of Fair Lawn, this complaint often leads to a more useful exam than patients expect. We look for plaque and tartar under the gumline, measure pocket depths, check for inflamed tissue, and rule out other causes such as decay or dry mouth. Sometimes the answer is straightforward gingivitis and a professional cleaning helps. Sometimes the odor is a warning sign that periodontal pockets are forming and deeper treatment is needed.
A better short list of next steps:
Mouthwash can freshen breath for a short time, but alcohol-heavy rinses may leave the mouth drier. Chewing gum may help briefly too, but it does not treat plaque, tartar, or gum infection. If breath odor is being driven by gum disease, the improvement usually comes from treating the source, not masking it.
A patient often notices this in the mirror before it hurts. One tooth looks longer than the one next to it, or a cold drink starts causing a quick, sharp zing near the gumline.
Gum recession means the edge of the gum has moved lower on the tooth, which can expose the root surface. In the severity ranking of gum disease signs, this sits beyond the earliest gingivitis changes because it can reflect loss of support, not just surface inflammation. Recession does not always mean periodontitis. Brushing too hard, clenching, tooth position, and thin gum tissue can all contribute. The important part is figuring out which cause is driving it.

Roots are more sensitive than enamel-covered tooth surfaces. Once they are exposed, patients may notice discomfort with cold water, sweet foods, brushing, or even air. The area can also wear down faster and collect plaque more easily, which makes home care harder.
In practice, the trade-off becomes a key consideration. If the recession is mainly from brushing trauma, technique changes and a softer brush may slow or stop further damage. If active gum disease is involved, better brushing alone will not fix the deeper problem. The gum attachment and bone support need to be checked.
At Dental Professionals of Fair Lawn, we look at the pattern, not just the symptom. A single recessed tooth may point to brushing force, bite stress, or tooth position. Recession affecting several teeth, especially with bleeding, deeper pockets, or tartar below the gumline, raises more concern for periodontitis.
Some recession can be stabilized. Gum tissue usually does not return to its old position on its own.
Helpful next steps:
That last step matters more than patients expect. If you are planning whitening, bonding, aligners, crowns, or veneers, untreated recession can affect comfort, appearance, and long-term results. Stable gums come first.
A tooth that feels loose, drifts out of line, or starts opening a new gap usually points to a later stage of gum disease. By this point, the problem is no longer limited to irritated gum tissue. The bone and periodontal ligament that hold the tooth in place may already be breaking down.
Patients in Fair Lawn often describe this in practical terms. A front tooth no longer lines up with the one next to it. Biting into a sandwich feels different. Floss slides through a space that was not there a few months ago.
This sign matters because it changes the treatment discussion.
With early gingivitis, treatment focuses on reducing inflammation and improving home care. With tooth mobility, we also have to ask how much support remains, whether bite pressure is making the problem worse, and whether the tooth can still be kept stable over time. Some loose teeth can be treated and monitored. Others have lost too much support, and keeping them may work against the health of nearby teeth.

At Dental Professionals of Fair Lawn, we check more than whether a tooth moves. We measure how much it moves, look for bone loss on imaging, evaluate the gums around it, and check whether clenching or an uneven bite is adding extra force. That combination helps determine whether the tooth is a candidate for periodontal treatment, temporary splinting, or replacement planning.
Helpful next steps:
Pain is not a reliable guide here. Some patients have very little discomfort even when support has been lost. If a tooth feels mobile or looks like it is changing position, get it checked promptly. At this severity level, early action can make the difference between stabilizing the tooth and planning for extraction and replacement.
A common mid-stage warning sign sounds like this: “My teeth don’t line up the same way,” or “My partial suddenly feels loose at dinner.” Patients often notice the bite before they notice the gums.
If your bite feels different, something underneath may have changed. Gum disease can weaken the bone and ligament support around teeth, and that can alter how your teeth meet. With dentures or partials, the fit can change when the gums and jaw ridge no longer support the appliance the same way they did before.
Sometimes the fix is a simple adjustment. Sometimes adjusting the appliance only masks a larger periodontal problem for a short time. That trade-off matters. A denture that rubs because of a sore spot is different from a denture that rocks because the underlying tissues or nearby teeth have changed.
We see this in practical ways at Dental Professionals of Fair Lawn. A patient may say the partial feels stable in the morning but shifts while chewing. Another may notice that one side touches first when they close. Those details help us decide whether the issue is wear in the appliance, tooth movement, gum inflammation, bone loss, or a combination of factors.
What to do:
This sign ranks higher in severity than bleeding or bad breath because it can reflect structural change, not just surface inflammation. It does not always mean an emergency, but it does mean the problem has moved beyond early gingivitis and deserves a closer exam soon.
You bite down on one side and feel a sudden, sharp pressure near the gumline. Later, you notice a small bump, a bad taste, or drainage near the tooth. That pattern can point to a periodontal abscess, and it needs prompt care.
Pus near the gums means infection is active, not just irritation. By the time this sign appears, the problem has usually moved past early gingivitis and into a more serious stage of gum disease. Pain can be strong, but sometimes the first clue is pressure, swelling, or a foul taste rather than severe pain.
This sign ranks near the top of the severity scale because infection can spread through the gum tissue and around the supporting structures of the tooth. Home care may keep the area cleaner, but it will not remove trapped bacteria, calculus, or infected debris below the gumline. If your treatment plan includes periodontal therapy after the urgent infection is controlled, our guide to when deep cleaning the teeth is recommended explains what that care involves.
Warm salt water rinses may reduce irritation for a short time. Pressing on the swelling, poking it with a sharp object, or waiting for it to drain on its own can make the area more inflamed and delay proper treatment.
What to do:
What not to do:
At Dental Professionals of Fair Lawn, we treat the immediate problem first, then check the surrounding gums, bone support, and tooth condition to see why the abscess formed. That trade-off matters. Relieving pressure helps you feel better quickly, but lasting improvement depends on treating the source of the infection, not only the flare-up.
A patient can have very little pain and still have worsening gum disease. Deep periodontal pockets are one of the clearest examples. You usually cannot see them in the mirror, but they often tell us more about disease severity than surface redness or bleeding alone.
During an exam, the dentist or hygienist measures the space between the tooth and gum with a periodontal probe. Healthy gums tend to fit more closely around the tooth. As infection and inflammation progress, that space deepens. The deeper it gets, the easier it is for plaque, bacteria, and hardened buildup to stay trapped below the gumline.
Pocket depth also helps separate early, reversible gum inflammation from more advanced periodontitis. Once pockets deepen, home brushing and flossing may still help control new plaque above the gums, but they cannot reliably clean the infected root surface underneath. That trade-off is important for patients to understand. Good home care still matters, but it may not be enough by itself.
If your measurements are increasing, treatment usually shifts from routine preventive care to periodontal therapy. Our guide to when deep cleaning the teeth is recommended explains how scaling and root planing fits into that plan.
A short video can also help make pocketing easier to understand:
At Dental Professionals of Fair Lawn, we use periodontal charting and imaging to track these changes over time, especially for patients in Fair Lawn, NJ who feel their gums are "mostly fine" but have risk factors or past disease. That matters because deep pockets sit near the severe end of these 8 warning signs. They often mean the problem has moved beyond gingivitis and needs prompt, structured treatment rather than watchful waiting.
| Sign | Detection complexity | Resource requirements | Expected outcomes / implications | Ideal response / use case | Key advantages |
|---|---|---|---|---|---|
| Red, Swollen, or Tender Gums | Low, visible on self‑exam or routine check | Minimal, visual exam, basic oral hygiene tools | Early inflammatory stage; often reversible with timely care | Improve home hygiene, schedule professional cleaning, monitor | Early, visible warning sign that prompts intervention |
| Bleeding Gums During Brushing or Flossing | Low, easily observed during hygiene | Minimal, patient self‑monitoring; dental exam if persistent | Indicates active inflammation; predicts need for treatment | Continue gentle flossing, seek pro cleaning if persistent >1 week | Objective, easy‑to‑track indicator that motivates care |
| Persistent Bad Breath or Mouth Odor | Moderate, subjective, may be missed by patient | Moderate, periodontal assessment, interdental cleaning tools, possible antimicrobial therapy | Persistent halitosis often reflects bacterial load and deeper pockets | Periodontal evaluation, targeted cleaning, adjunctive antimicrobials | High patient motivation; improvement tracks treatment success |
| Gum Recession / Exposed Tooth Root | Moderate, visible but cause assessment needed | Moderate–high, clinical exam, imaging, possible surgical consult | Sign of tissue/bone loss; may be irreversible; increases sensitivity/decay risk | Preventive measures, desensitizing care, consider grafting or restorative options | Clear indicator of structural damage guiding definitive care |
| Loose or Shifting Teeth | Moderate–high, clinical mobility tests and bite assessment | High, comprehensive perio exam, radiographs, stabilization or surgical resources | Reflects advanced bone loss; elevated risk of tooth loss | Urgent professional evaluation, stabilization, salvage or replacement planning | Strong marker of severity; measurable and action‑prompting |
| Changes in Bite or Fit of Dentures/Partials | Moderate, patient reports plus clinical fit checks | Moderate–high, denture adjustment, perio assessment, prosthetic services | Indicates jaw/tooth support changes from periodontal disease | Immediate dental review, relining/adjustment, consider implant options | Functional sign that reveals impact on prosthetics and occlusion |
| Pus or Abscess Formation Between Teeth and Gums | Low, often visible and symptomatic (pain/swelling) | High, emergency drainage, antibiotics, possible surgery | Active infection; medical emergency with risk of spread | Same‑day emergency dental care, incision/drainage, systemic therapy | Clear urgent sign requiring prompt intervention for rapid relief |
| Deep Periodontal Pockets / Increased Probing Depth | High, requires calibrated probing and charting | High, periodontal probing, charts, radiographs, possible advanced therapy | Objective diagnostic criterion for disease stage and progression | Professional scaling/root planing, frequent monitoring, surgical options if deep | Gold‑standard measurable marker for diagnosis and treatment planning |
You book a visit for a cosmetic concern, or because food keeps catching between two teeth, and the underlying issue turns out to be your gums. That happens often. Gum disease does not always announce itself with strong pain, which is why this 8-sign list matters most when you use it to judge urgency.
The first few signs on this list, such as redness, tenderness, or bleeding, often point to gingivitis. At that stage, treatment is usually simpler and aimed at stopping inflammation before support around the teeth starts to break down. The later signs, such as loose teeth, pus, and deeper pockets, point to periodontitis and call for faster, more involved care.
As noted earlier, the CDC’s overview of gum disease shows that periodontal disease is common in adults and more likely in patients with risk factors such as smoking and diabetes. In practice, that means feeling "mostly fine" is not a reliable way to rule it out.
Home care still matters. Brushing well twice a day, cleaning between the teeth, and keeping regular recall visits can reduce inflammation and help keep early disease from getting worse. Home care cannot remove tartar below the gums, measure pocket depths, or treat an abscess. If you have reached the middle or upper end of this severity list, waiting usually limits your options.
That is the trade-off patients should understand. Early treatment is often less invasive, less expensive, and easier to recover from. Delayed treatment may require scaling and root planing, periodontal maintenance, surgical treatment, tooth stabilization, or decisions about replacement if support has already been lost.
At Dental Professionals of Fair Lawn, the next step is a focused periodontal evaluation based on what your gums are doing now, not a one-size-fits-all plan. That may include charting pocket depths, checking for bleeding, reviewing X-rays, and matching treatment to the severity of the signs you noticed. If anxiety has kept you from coming in, say so at the start. We can work through that more effectively when we know it upfront.
If you recognized your symptoms in the lower-severity signs, schedule an exam soon. If you recognized the higher-severity signs, especially pus, swelling, shifting teeth, or a bite that feels different, get seen promptly.
If you’re looking for a Dental Professionals of Fair Lawn appointment for bleeding gums, bad breath, gum recession, loose teeth, or a full periodontal evaluation, contact the office to schedule a visit. The team serves Fair Lawn, Ridgewood, Glen Rock, and nearby New Jersey communities with preventive, restorative, cosmetic, implant, orthodontic, emergency, and advanced periodontal care.