Don't Ignore These Signs You Need Your Wisdom Teeth Removed
Experiencing jaw pain? Learn the 8 key signs you need your wisdom teeth removed. Our Fair Lawn pros offer expert extraction. Schedule now.
Experiencing jaw pain? Learn the 8 key signs you need your wisdom teeth removed. Our Fair Lawn pros offer expert extraction. Schedule now.
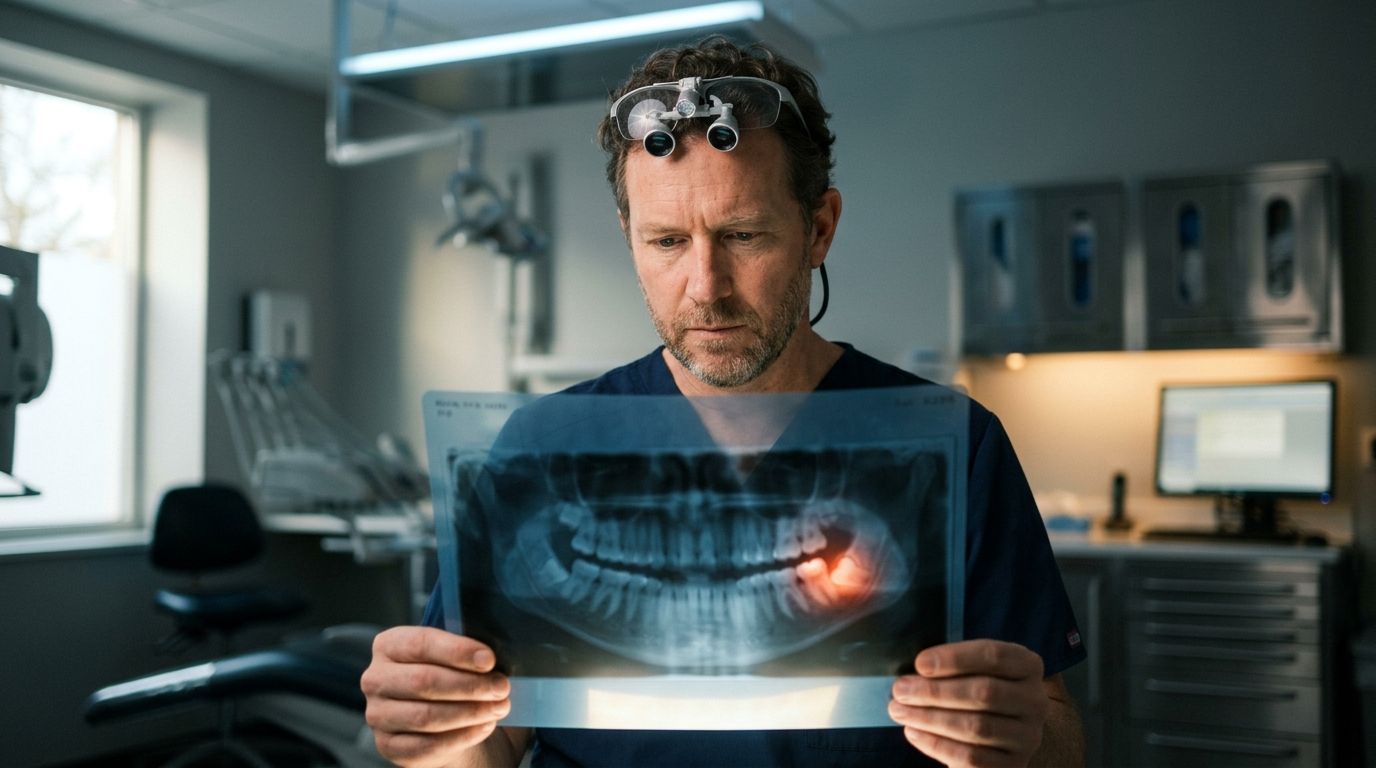
You wake up with pressure near the back of your jaw, chew on one side to avoid it, and notice the tissue behind your last molar feels irritated again. That is often how wisdom tooth trouble starts. The change is subtle at first, then it keeps returning.
For patients in Fair Lawn, Ridgewood, and Glen Rock, the question is rarely whether a symptom is annoying. Rather, the question is what is causing it, and whether the tooth can be monitored safely or is starting to threaten the gum, bone, or neighboring molar. Wisdom teeth often begin causing problems in the late teen and young adult years, but the timing and severity vary from person to person.
Some wisdom teeth erupt normally and stay easy to clean. Others remain trapped under the gums, come in at an angle, or open just enough to collect bacteria and food. Clinical guidance on common indicators for wisdom teeth removal includes pain, swelling, crowding, infection, decay, jaw stiffness, and sinus-related pressure. Those symptoms matter, but symptoms alone do not tell the whole story.
At Dental Professionals of Fair Lawn, Dr. Jody Bardash evaluates wisdom teeth with the same focus we use for any surgical decision. We look at your exam, your bite, and the position of the tooth on imaging. Facial scanning helps us assess how the jaw and surrounding structures are relating clinically. CBCT gives a three-dimensional view when we need to see the exact angle of an impacted tooth, its proximity to nerves or sinuses, and whether bone loss, infection, or a cyst is developing around it.
That information shapes the treatment plan. Some patients need monitoring and better home care. Some benefit from early removal before the roots become more difficult to manage. If extraction is the right choice, we can discuss sedation for comfort, oral surgery planning for impacted teeth, and bone grafting when preserving the site or supporting long-term oral health makes sense.
The signs below explain when wisdom teeth move from harmless to harmful, and what each finding means in a real dental setting.
Pain is still the symptom that often brings individuals in first. Sometimes it’s sharp and obvious. Sometimes it’s a low-grade ache that comes and goes for weeks, then flares when you chew, yawn, or brush near the back teeth.
That pattern matters. Wisdom teeth often create pressure in the far back of the mouth, especially when they’re partially erupting or pushing at an angle. Clinical descriptions of removal warning signs specifically note persistent pain and discomfort as a common reason for extraction, including pain that can radiate into the jaw, ear, or neck.

A patient might say the area “just feels sore” until they eat something crunchy. Another might feel a stabbing pain only when the tooth starts breaking through the gums. Others notice tenderness that spreads toward the ear and makes the whole side of the jaw feel tired.
Pain from wisdom teeth doesn’t always mean the tooth must be removed that day. But it does mean the area needs a proper exam. Temporary relief from ibuprofen, soft foods, or rinsing doesn’t solve the reason the pain keeps returning.
Practical rule: If pain in the back of your mouth keeps coming back, it’s time for imaging, not guesswork.
At Dental Professionals of Fair Lawn, that evaluation may include digital X-rays and, when the position is more complex, a CBCT scan to see root shape, bone support, and nearby structures clearly. That’s especially helpful when a tooth is impacted and the visible part of the problem is much smaller than the hidden part.
A few simple steps can keep you more comfortable while you wait for your visit:
If you’re also dealing with swelling, limited opening, or a bad taste, that moves the problem from uncomfortable to urgent faster than many people expect.
Some wisdom teeth don’t hurt much at first. They swell first. You may notice puffiness behind the last molar, tenderness in the gum, or a cheek that looks slightly fuller on one side when you look in the mirror.
That kind of inflammation often means the tooth is trapped under tissue, erupting at an awkward angle, or collecting bacteria in an area that’s hard to clean. Red, tender gums, facial swelling, and even difficulty opening the mouth fully are recognized warning signs when wisdom teeth are creating trouble.
This is one reason people delay care. The swelling may calm down for a few days, then return after chewing, poor sleep, stress, or food getting trapped under the gum flap around a partially erupted tooth. Patients sometimes assume that if the swelling went down, the problem is gone.
Usually it isn’t. The tissue may be less irritated for the moment.
In younger patients, swelling may show up as mild gum puffiness during eruption. In adults, chronic inflammation is more likely to signal a partially impacted wisdom tooth that has become a repeated source of irritation. If swelling is visible in the cheek or jawline, I take that seriously because deeper inflammation is often involved.
You can support the area, but you shouldn’t try to manage ongoing swelling indefinitely at home.
Swelling that keeps returning is your mouth’s way of saying the area isn’t stable.
At Dental Professionals of Fair Lawn, facial scanning and digital imaging help us compare what you feel externally with what’s happening internally. If the issue is simple gum irritation, monitoring may be enough. If the wisdom tooth is positioned badly or creating repeated inflammation, removal is often the cleaner long-term solution.
This concern often comes from patients who’ve already put time into their smile. They’ve had braces, completed Invisalign, or worn retainers faithfully, then suddenly the lower front teeth start feeling tighter or the bite seems slightly off. The wisdom teeth become the first suspect.
Crowding around the back teeth is a real issue when there isn’t enough room for eruption. Clinical guidance lists crowding of adjacent teeth, shifting, overlapping, and crooked alignment among the signs that wisdom teeth may need removal.
Patients don’t usually come in saying, “I think my third molars are impacted.” They say, “My teeth were straight, and now they feel different.” That’s a useful clue.
Wisdom teeth are the last molars to erupt, and late eruption pressure in a tight jaw can create problems at the back of the arch. Even when they aren’t the only factor in shifting, they can make a crowded situation harder to manage. I’m especially cautious when someone has finished orthodontic treatment and now feels pressure behind the second molars.

Not every change in alignment means wisdom teeth are the sole cause. But these patterns deserve an exam:
If you’ve had Invisalign, Damon treatment, Six Month Smiles, or traditional braces, this conversation matters. The goal is to protect the result you worked for, not just to react once the crowding becomes obvious.
A good diagnostic visit should answer three questions clearly. Is there enough room? Are the wisdom teeth erupting in a healthy path? Are they threatening the neighboring molars or your bite? If the answer to those questions points toward future damage, removal may be the more conservative choice in the long run.
Some wisdom teeth don’t announce themselves with severe pain. They create a daily nuisance instead. Food packs into the back corner. Floss shreds. Your toothbrush never seems to reach fully. The area smells off even after you brush carefully.
That matters because a tooth you can’t clean well is a tooth that often becomes a recurring source of inflammation, decay, and bad breath.
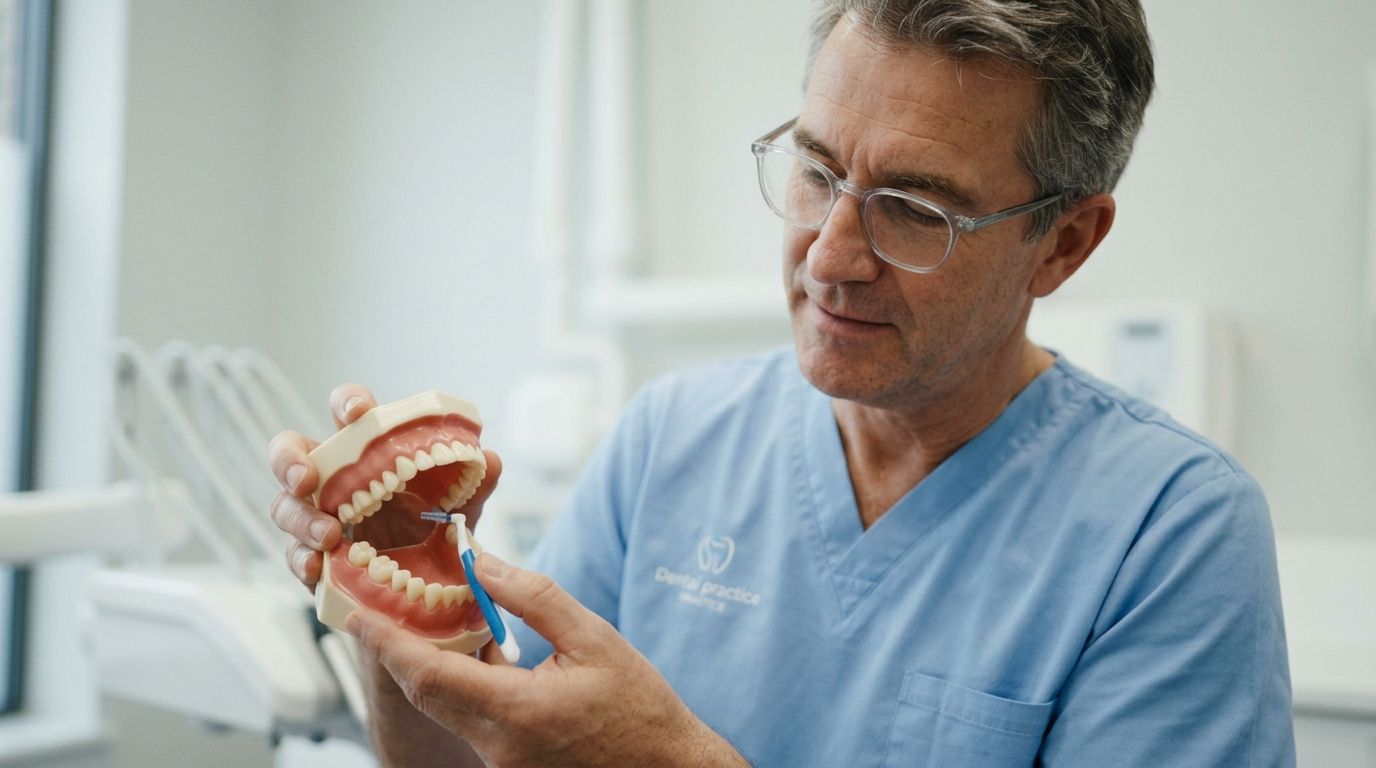
I always distinguish between “needs better brushing” and “physically difficult to access.” Those are not the same thing. A partially erupted wisdom tooth can leave a pocket under the gum or behind the second molar that traps plaque and debris no matter how conscientious you are.
That’s why some patients with excellent hygiene still end up with repeated problems around wisdom teeth. The issue isn’t effort. It’s anatomy.
Fully erupted, healthy, and properly aligned wisdom teeth might not require removal if they can be cleaned and monitored consistently. But if the area remains hard to reach and keeps getting inflamed, retention stops being a practical plan.
Before a definitive decision, a few tools can make a real difference:
This short demonstration can help patients understand technique, especially in hard-to-reach back areas.
If careful home care, regular cleanings, and better tools still don’t keep the area healthy, extraction is often the more predictable solution. In those cases, leaving the tooth in place tends to create repeat visits for the same problem.
This is one of the quieter reasons wisdom teeth come out. You may feel nothing at all, and the problem is still serious. A cyst or tumor associated with an impacted wisdom tooth is often found on imaging before the patient notices symptoms.
Clinical guidance specifically includes cyst or tumor formation near wisdom teeth as a warning sign because these lesions can damage surrounding jawbone and nearby structures if they aren’t treated.
A buried wisdom tooth can look uneventful during a routine visual exam. But when we take digital X-rays or a CBCT scan, we sometimes find a darkened area around the tooth that suggests a pathologic change in the surrounding tissue. That’s where advanced imaging becomes more than a convenience. It becomes a safeguard.
Patients are often surprised because the area didn’t hurt. But symptom-free doesn’t always mean harmless. If a cyst enlarges, it can weaken bone, affect adjacent teeth, and complicate treatment.
Healthy-looking gums do not rule out a deeper wisdom tooth problem.
At Dental Professionals of Fair Lawn, detailed surgical planning is essential. If the wisdom tooth and surrounding lesion need to be removed, the treatment may fall within oral surgery at Dental Professionals of Fair Lawn, especially when the tooth is impacted or the site may need additional reconstruction.
Not every radiographic finding means the same thing. Some areas need removal right away. Others need prompt evaluation to determine the safest next step. In larger defects, bone grafting may be part of the treatment plan after extraction so the area heals with better support.
Patients usually do best when this is caught early, before the lesion has expanded enough to damage more tissue. That’s another reason routine exams and updated imaging matter, even if you aren’t in pain. The goal is to solve the problem while treatment is still straightforward.
Upper wisdom teeth sit close to the maxillary sinus, so problems there can create symptoms people don’t immediately connect to dentistry. They describe pressure in the cheek, headaches behind the eyes, or one-sided fullness that feels like a sinus issue but doesn’t completely behave like one.
Sinus problems and jaw stiffness are included among the warning signs associated with problematic wisdom teeth, particularly when the teeth are misaligned or impacted.
A careful history helps. If a patient tells me the pressure is mostly on one side, worsens near the upper back molars, or comes with chewing discomfort, wisdom teeth move higher on the list of possibilities. I don’t assume every headache is caused by third molars, but I also don’t ignore that connection.
A common scenario is the patient who has recurring facial pressure and tenderness over one upper posterior area, yet the pattern never fully resolves. Imaging can show whether the roots are close to the sinus floor or whether the tooth is impacted in a way that may be contributing to the irritation.
Diagnosis matters because this symptom overlaps with other conditions. TMJ strain, sinus disease, clenching, and bite problems can all create similar discomfort.
At our Fair Lawn office, a CBCT scan can be especially useful when sinus anatomy and tooth position need to be assessed together. Facial scanning and a bite evaluation may also help if headaches seem tied to jaw tension rather than the sinus itself. The right answer isn’t always extraction. But when an upper wisdom tooth is clearly part of the problem, removing it can eliminate a source of recurring pressure and inflammation.
A patient may come in with a small cavity on a wisdom tooth and assume it is a simple filling. Often, it is not. These teeth sit so far back that decay is usually tied to poor access, partial eruption, or an angle that keeps trapping food and bacteria. In many cases, the second molar in front of the wisdom tooth starts breaking down as well.
That changes the decision. The question is no longer whether the wisdom tooth can be repaired. The better question is whether keeping it puts a healthier, more useful tooth at risk.
I look at more than the cavity itself. If I cannot get a clear, dry working area, if the tooth has little value in your bite, or if the position keeps creating the same problem, a filling may only delay the next issue. Patients deserve a practical answer, not temporary dentistry in a hard-to-maintain area.
At Dental Professionals of Fair Lawn, facial scanning and CBCT imaging help show exactly how the wisdom tooth is sitting, whether decay has reached the second molar, and whether removal can be done in a controlled way. That matters because treatment planning is different when the goal is protecting the neighboring molar, preserving bone, and making the procedure easier on the patient. If anxiety or a difficult impaction is part of the picture, sedation and oral surgery can be planned from the start, not added as an afterthought.
These are common warning signs:
If you are also seeing inflammation or bleeding in that area, it can help to compare those symptoms with common warning signs of gum disease, especially when it is not clear whether the problem is decay, gum irritation, or both.
If a wisdom tooth keeps damaging the tooth in front of it, removal is often the more conservative choice.
We also plan for what comes after extraction. Some patients only need the wisdom tooth removed. Others need a filling on the second molar, close monitoring of the area, or bone grafting if the defect behind that tooth is deeper than expected. Managing the diagnosis, extraction, and restorative follow-up in one office helps protect the rest of your smile with fewer delays and fewer surprises.
If you notice pus, drainage, a foul taste, severe tenderness, or swelling around a partially erupted wisdom tooth, that’s not something to monitor casually. This often points to pericoronitis, an infection in the gum tissue around the tooth.
Partially erupted wisdom teeth create an ideal environment for bacterial buildup, and recurrent infections around them are a well-recognized reason for removal.
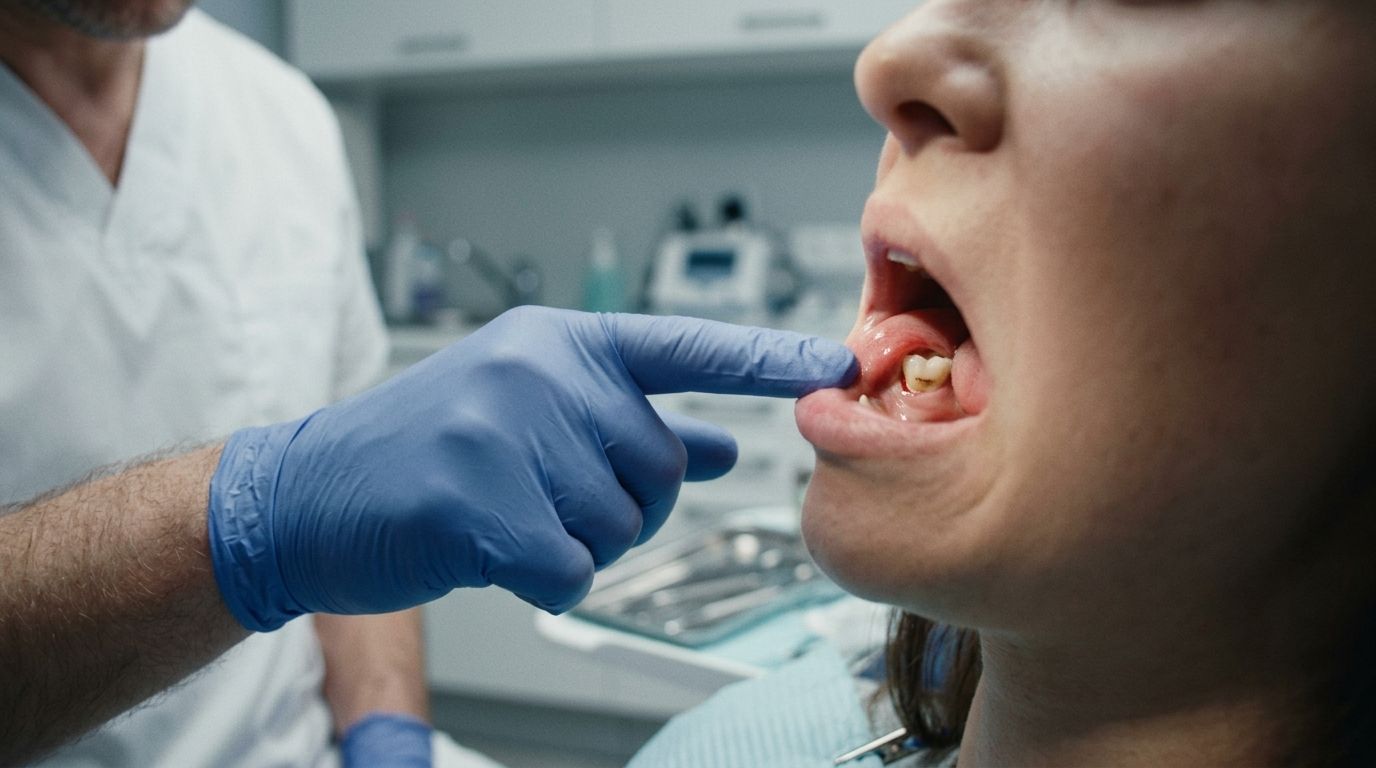
Sometimes it starts with a bad taste that won’t go away. Sometimes it’s tenderness under a gum flap, followed by swelling and difficulty chewing. In more advanced cases, the patient has trouble opening comfortably and feels that the whole side of the mouth is inflamed.
Because this can overlap with broader gum problems, some patients aren’t sure what they’re seeing. If you’ve had bleeding, tenderness, or inflammation in several areas of the mouth, it can also help to understand the warning signs of gum disease. But when the problem is concentrated around a partially erupted wisdom tooth with drainage or foul odor, pericoronitis rises to the top of the list.
Home rinses may reduce surface irritation for a short time, but infection around a wisdom tooth usually returns unless the underlying issue is addressed. The treatment may involve cleaning the area, controlling active infection, and then planning extraction once it’s safe and appropriate.
Seek urgent dental care if you notice any of the following:
When patients ask me which sign matters most, infection is near the top. Pain is miserable. Crowding is frustrating. Active infection can escalate.
| Indicator | Implementation complexity | Resource requirements | Expected outcomes | Ideal use cases | Key advantages |
|---|---|---|---|---|---|
| Persistent pain or discomfort in the back of the mouth | Low–Moderate (clinical exam + imaging; often standard extraction) | Dental exam, X-rays/CBCT, possible surgical suite | Rapid pain relief after extraction; lowers complication risk | Recurrent or worsening posterior jaw/molar pain | Clear clinical trigger for evaluation; typically resolved by removal |
| Swelling or inflammation of the gums and jaw | Moderate (may need antibiotics then surgical extraction) | Imaging, antibiotics, periodontal assessment, possible surgery | Swelling reduction and infection control; improved jaw function | Visible facial/jaw swelling, limited mouth opening, suspected infection | Visible, urgent symptom prompting prompt care; extraction often resolves inflammation |
| Crowding of other teeth or misalignment | Low–Moderate (timing coordination with orthodontics) | Orthodontic consult, imaging, planned extraction | Preservation of orthodontic results; prevention of future relapse | Teens, post-orthodontic patients, early signs of shifting | Preventive protection of smile alignment and orthodontic investment |
| Difficulty cleaning behind the last molars | Low (hygiene strategies or preventive extraction) | Interdental tools, frequent cleans, imaging, possible extraction | Reduced decay and gum disease risk; easier oral hygiene | Persistent food trapping, recurrent posterior decay despite care | Eliminates hard-to-clean niches; improves long-term oral hygiene |
| Cyst or tumor development around impacted teeth | High (surgical extraction, possible grafting, specialist care) | Advanced imaging, oral surgery, bone grafting capability | Removal of pathology; prevents bone loss and structural damage | Imaging-detected cysts/lesions or expanding radiolucencies | Addresses underlying pathology and prevents major jaw complications |
| Sinus problems or headaches linked to wisdom teeth | Moderate–High (interdisciplinary evaluation often needed) | Dental and sinus imaging, ENT coordination, surgical extraction | Gradual reduction in sinus congestion and headache frequency | One-sided sinus symptoms or recurring headaches near molars | Can resolve chronic sinus/headache issues related to tooth impaction |
| Decay or cavities in wisdom teeth or adjacent molars | Moderate (assess restoration vs extraction; treat infection first if present) | Restorative treatment options, imaging, possible extraction | Eliminates recurrent decay source; protects second molars | Recurrent posterior cavities or extensive decay hard to restore | Often more cost-effective than repeated restorations; protects adjacent teeth |
| Pus, discharge, or infection around wisdom teeth (pericoronitis) | High urgency (may require emergency antibiotics then extraction) | Emergency dental care, antibiotics, possible hospital support | Rapid infection control; prevents systemic spread and complications | Active infection with pus, fever, swelling, or difficulty swallowing | Immediate source control and infection resolution; prevents serious progression |
You feel pressure behind your last molar when you chew, then one morning the gum is swollen again. That pattern is usually a sign to stop guessing and get a clear look at what the tooth is doing.
Wisdom teeth are common. Removal is not automatic. Some third molars come in straight, stay clean, and can be monitored. Others stay partly trapped under the gums or bone, collect bacteria, press against the second molar, or trigger repeated pain and swelling. Those teeth rarely become simpler with time.
The next step is an exam that answers two questions. Is the tooth healthy enough to keep, and if not, what is the safest way to remove it? At Dental Professionals of Fair Lawn, Dr. Jody Bardash starts with your symptoms, your bite, and the condition of the gum tissue around the area. Digital X-rays help with many cases. If the position of the tooth is unclear, or if roots appear close to the nerve or sinus, CBCT imaging gives a three-dimensional view of the tooth, surrounding bone, and nearby anatomy so treatment decisions are based on detail rather than estimates.
That imaging matters. A patient with intermittent soreness may only need monitoring, while a patient with an impacted tooth pressing into the second molar may be better served by earlier removal before decay, infection, or bone loss develops. Facial scanning and advanced imaging also help us explain what is happening in a way patients can see, which makes the decision easier and more grounded.
Comfort is part of the plan too.
Patients often delay wisdom tooth treatment because they expect a difficult appointment. In practice, the experience depends on the position of the tooth, the amount of inflammation present, and the level of anxiety involved. Sedation options can make treatment far more manageable, especially for impacted extractions or for patients who have had stressful dental visits in the past. The goal is not only to remove the tooth. It is to do it in a controlled, calm setting with a recovery plan that makes sense for your case.
Some cases need more than a straightforward extraction. If a wisdom tooth has damaged the tooth in front of it, restorative treatment may be part of the plan. If an impacted tooth leaves a defect in the jaw, bone grafting may help support better healing and preserve the area. Keeping diagnosis, oral surgery, sedation, and follow-up care coordinated in one office can spare patients the confusion of trying to piece treatment together across multiple locations.
If you live in Fair Lawn, Ridgewood, Glen Rock, or a nearby community and these symptoms sound familiar, the next useful step is an evaluation. You may learn your wisdom teeth can be watched safely. You may learn removal is the better choice. Either way, you leave with a clear diagnosis and a treatment plan built around your comfort and long-term oral health.
If you’re dealing with jaw pain, swelling, crowding, infection, or you want a trusted dentist in Fair Lawn, NJ to evaluate your wisdom teeth, schedule a visit with Dental Professionals of Fair Lawn. Dr. Jody Bardash and the team provide thorough exams, dental X-rays, CBCT imaging, sedation options, tooth extraction care, and complete follow-up treatment in one welcoming office serving Fair Lawn, Ridgewood, Glen Rock, and nearby communities.