Can Small Cavities Go Away? Expert Answers Here
Want to know if can small cavities go away on their own? Find out when tooth decay can reverse and when to see a dentist in Fair Lawn, NJ for treatment.
Want to know if can small cavities go away on their own? Find out when tooth decay can reverse and when to see a dentist in Fair Lawn, NJ for treatment.
You spot a tiny white mark near the gumline, or maybe a dark speck in a groove on a back tooth. It doesn’t hurt. You search can small cavities go away because you’re hoping the answer is yes, and also because you’re worried it might turn into something bigger.
That question is more common than one might assume. Many people in Fair Lawn, Ridgewood, and Glen Rock notice a small change in a tooth and aren’t sure whether they should watch it, brush better, or book an exam right away. The confusing part is that both “yes” and “no” can be true, depending on what stage the tooth is in.
A very early weak spot in enamel may improve. A true hole in the tooth won’t heal on its own. Knowing the difference matters, because it can mean the difference between a conservative treatment and a more involved repair later.
A patient often notices the problem in an ordinary moment. Brushing before work. Looking in the mirror after lunch. Helping a child floss before bed. There’s a pause, then the same thought appears: “That wasn’t there before.”

Sometimes it’s a chalky white spot. Sometimes it’s a faint brown area in a groove. Parents often notice a mark on a child’s molar and wonder whether they’re overreacting. Adults do the same thing, especially if they haven’t had pain yet. That’s where confusion starts. People assume that if it doesn’t hurt, it must be minor. In dentistry, that isn’t always how decay works.
Many aren’t asking whether decay is technically reversible. They’re asking something more practical:
Those are fair questions. They deserve a clear answer, not a vague “it depends” with no explanation.
Small changes in a tooth don’t always mean you need drilling. But they do mean you need an accurate diagnosis.
That’s especially important for families trying to choose a dentist in Fair Lawn, NJ they can trust for routine care, cleaning and exams, dental x-rays, and new patient exams. A calm evaluation can tell you whether you’re looking at early enamel damage, a cavity that needs treatment, or something else entirely such as staining or wear.
A tiny spot can look harmless at home and still be active decay. The opposite can happen too. A mark that looks alarming in the mirror may turn out to be superficial staining or an area the dentist wants to monitor.
That’s why the smartest next step usually isn’t guessing. It’s getting an exam while the issue is still small. For patients searching dentist near me, emergency dentist, or even cosmetic dentist near me because they’re concerned about how a tooth looks, a professional assessment brings clarity fast and helps protect your smile before a minor problem grows.
The simplest answer to can small cavities go away is this. Early damage can sometimes be reversed. A true cavity cannot. The reason is physical. In one stage, the tooth surface is still intact. In the other, that surface has broken open.
A helpful way to picture it is to look at decay in two layers. First, minerals leave the enamel and create a weak spot under the surface. Dentists call that demineralization. Later, if the process keeps going, the enamel collapses and forms a real opening. That is cavitation.
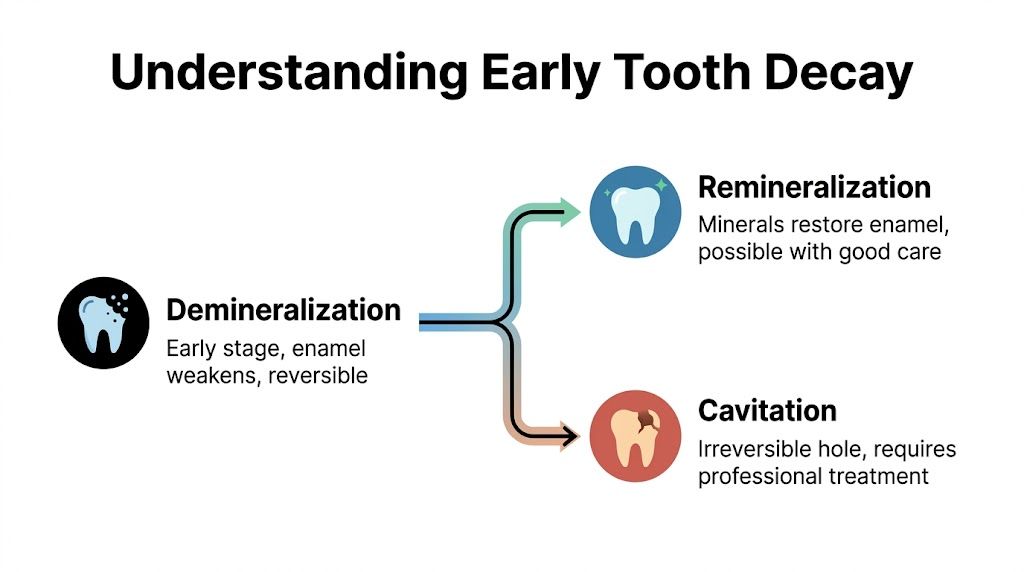
Your enamel is constantly losing and gaining minerals. After you eat or drink something sugary or acidic, plaque bacteria produce acid. If those acid attacks happen often enough, minerals begin leaving the enamel faster than saliva can replace them. The NIDCR explanation of the tooth decay process describes this early stage as subsurface demineralization. It also explains that fluoride helps enamel resist future acid damage.
This is why an early area of decay often looks like a chalky white spot instead of a brown hole. The surface can still be present even though the enamel underneath has started to soften.
That distinction matters.
If the outer surface remains intact, your dentist may be able to stop the area without drilling by strengthening the enamel, sealing the porous area, or using targeted treatments such as professional fluoride treatments for early enamel repair, resin infiltration, or SDF in the right situation.
Once the surface breaks, the tooth has lost structure. Saliva and fluoride can support the surrounding enamel, but they do not rebuild a missing piece of tooth the way your body can close a cut on your skin.
That is why online advice can sound contradictory. One source is talking about a weak spot. Another is talking about a hole.
Here is the practical difference:
| Stage | What is happening | Can it improve without drilling |
|---|---|---|
| Demineralization | Minerals have left the enamel, but the surface is still intact | Sometimes, yes |
| Cavitation | The enamel surface has opened into a physical hole | No |
A small dark mark is not always a cavity. A white spot is not always harmless. Some early lesions are active and spreading. Some are old areas that have hardened and stopped changing. Dry mouth can also speed up the process because saliva has less chance to buffer acid and return minerals to the tooth. If that sounds familiar, this guide to better nighttime breathing explains one common reason people wake up with a dry mouth.
The key takeaway is simple. Early spots may be reversible because the enamel surface is still there. True cavities do not go away because the tooth has already developed a hole. That is why a careful dental exam in Fair Lawn matters so much. It tells you which stage you are in, and whether a modern, non-invasive treatment may still be an option.
If your dentist identifies an early weak spot rather than a true cavity, what you do at home matters a great deal. Home care won’t repair a hole, but it can support remineralization when the enamel surface is still intact.

According to this explanation of early reversal and prevention, early-stage demineralization can be reversed in approximately 4 to 8 weeks with consistent fluoride use and optimal oral hygiene, preventing progression in up to 40% of cases. That same source explains that saliva helps redeposit calcium and phosphate into enamel before a physical hole forms, and that sealants can reduce molar cavity risk by 80%.
The goal is to make your mouth less friendly to acid and more supportive of enamel repair.
Some people are doing many things right and still keep developing weak spots because their mouth is dry at night. Mouth breathing, snoring, and poor sleep habits can reduce the protective effect of saliva. If you wake up with a dry mouth often, this guide to better nighttime breathing offers useful context on why that happens.
Professional support can strengthen your efforts at home. If your dentist recommends in-office fluoride, learn more about fluoride treatments and when they’re used.
A quick visual can help reinforce the daily habits that protect enamel:
Home care is powerful, but it has limits. It can improve the environment in your mouth. It cannot tell you whether a spot is active, arrested, or already cavitated.
That’s where people lose time. They brush harder, switch toothpaste, cut back on sweets, and assume the problem is improving because the tooth doesn’t hurt. Sometimes they’re right. Sometimes the cavity is getting deeper unnoticed.
If you’re trying to reverse an early area, home care works best as part of a plan your dentist is monitoring.
There’s a point where trying to manage things at home stops being the safe choice. If you notice symptoms that suggest the enamel may already be broken, it’s time to look for a dentist near me for a cavity rather than hoping the tooth settles down on its own.
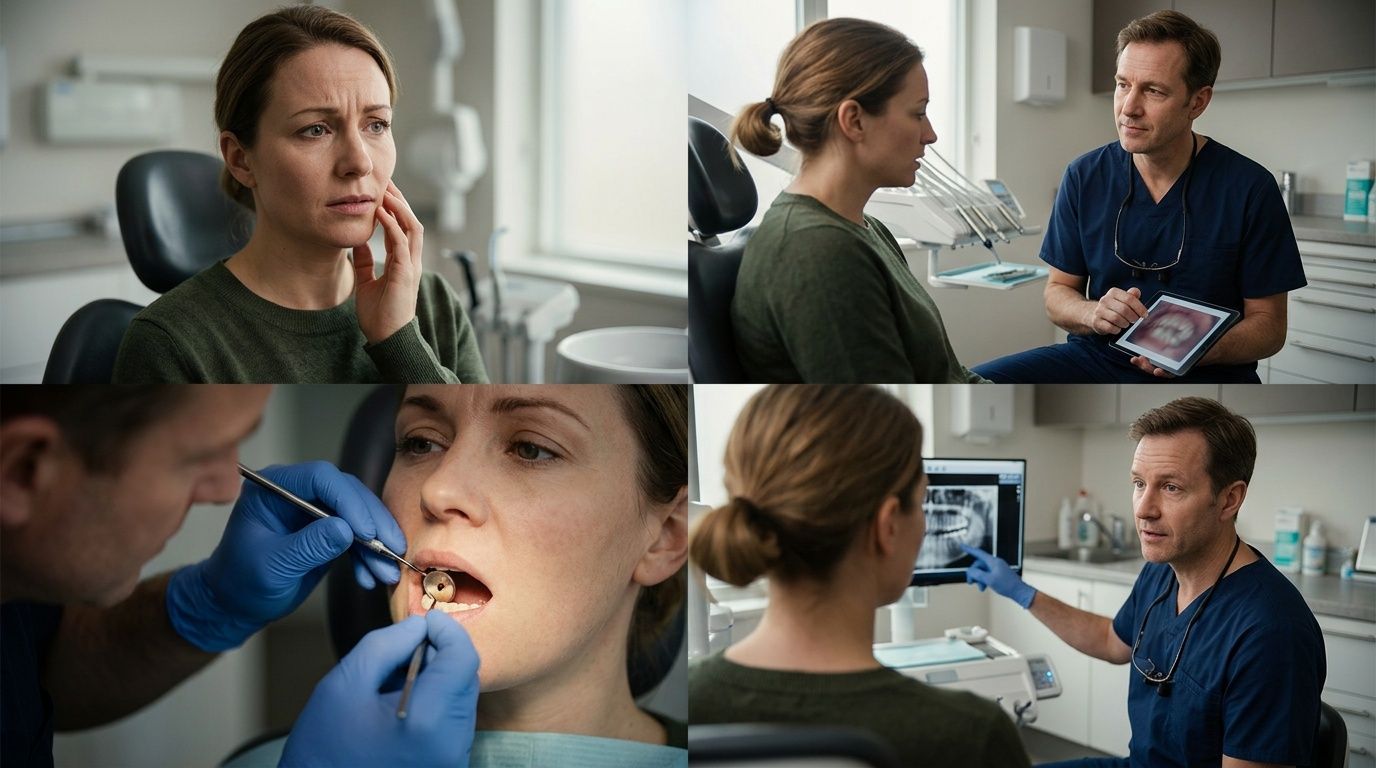
The reason is simple. This review of untreated cavity progression notes that untreated cavities can progress from small enamel lesions to severe infections in 6 to 24 months, and that 10% of U.S. adolescents ages 12 to 19 have at least one untreated cavity. The same source explains that true cavities, meaning physical holes, do not self-heal, while early detection with digital scanning can identify problems before they need more extensive restorative care.
Some signs suggest the problem may be beyond the reversible stage:
One symptom alone doesn’t confirm a cavity. But a pattern should not be ignored.
A lot of patients assume pain is the deciding factor. In reality, a cavity may cause no pain early on, or the pain may come and go. Sensitivity that disappears for a while doesn’t always mean the tooth healed. It may mean the inflammation shifted or the cavity changed.
That’s why a visual exam matters. If you’ve ever wondered whether a hidden area between teeth could be the reason a tooth feels “off,” this article on hidden tooth decay explains how problems can develop where you can’t easily see them.
If you can already see a hole, the question is no longer “can small cavities go away.” The better question is how to treat the tooth conservatively before the damage spreads.
If you have swelling, significant pain, or trouble chewing on one side, don’t wait. That’s when many people start searching for an emergency dentist or tooth extraction options. In some cases, prompt treatment can still save the tooth with a simpler restoration. Waiting may push the tooth into needing more involved restorative dentistry such as a crown or root canal.
Many people still picture cavity treatment as one path only. Numb the tooth, drill the decay, place a filling. That approach is still appropriate in many cases, but it’s not the only option for early decay.
For selected small lesions, dentists now have more conservative ways to stop the problem before it becomes a larger repair. That matters for children, anxious patients, and adults who want to preserve as much natural tooth structure as possible.

If a weak area is still non-cavitated, fluoride varnish may help arrest it. This is different from ordinary brushing because the dentist places a concentrated fluoride product directly on vulnerable enamel. It’s often used for children and adults who are at higher risk for decay.
Sealants work differently. They cover deep grooves on molars where plaque tends to collect. Instead of trying to rebuild enamel, they create a protective barrier over areas that are difficult to clean well.
This is one of the least discussed options online, yet it can be a very useful one for the right case. Resin infiltration for small cavities is a no-drill treatment designed for early decay before a true hole has formed. A low-viscosity resin flows into porous enamel after the surface is prepared, helping seal out acids and bacteria while preserving healthy tooth structure.
This option is especially appealing when the goal is to be conservative. It can also help patients who feel nervous about traditional drilling.
Another important option is Silver Diamine Fluoride, often called SDF. According to this overview of Silver Diamine Fluoride and no-drill options, SDF can arrest 80% of small cavities from progressing and is applied in about one minute. The same source explains that resin infiltration is an FDA-approved approach that seals early decay by flowing low-viscosity resin into enamel pores.
SDF can be especially helpful for:
There is an important cosmetic tradeoff. SDF can darken the treated decay. For back teeth or temporary management, that may be acceptable. For visible front teeth, many patients prefer other options.
Dentists don’t choose among these treatments by preference alone. They look at the location of the lesion, whether the surface is intact, your cavity risk, your age, the tooth involved, and whether you need a treatment that prioritizes appearance.
A short comparison shows the logic:
| Option | Best for | Main benefit | Main limitation |
|---|---|---|---|
| Fluoride varnish | Early weak enamel | Supports remineralization | Won’t close a hole |
| Sealant | Deep grooves on molars | Protects vulnerable pits and fissures | Not used for every lesion |
| Resin infiltration | Early smooth-surface or interproximal lesions | No-drill sealing of porous enamel | Not for larger cavities |
| SDF | Arresting small active decay | Very fast, conservative | Can darken treated areas |
The larger point is reassuring. Early diagnosis creates more choices. If you wait until the tooth has broken down further, those conservative options may no longer be appropriate.
A dental visit feels easier when you know what will happen. If you’re coming in because of a suspicious spot, sensitivity, or a tooth that just doesn’t seem right, the first step is gathering clear information.
The exam usually starts with a conversation. You describe what you noticed, when it started, and whether anything makes it worse. Small details help. Does cold trigger it? Is it one exact tooth? Did you notice a white spot or a dark groove? That history often tells the dentist where to focus.
Then comes the clinical exam. The dentist checks the enamel surface, the grooves of the molars, the gumline, and the contact points between teeth. If needed, dental x-rays help reveal decay that can’t be seen directly.
Modern offices may also use advanced imaging such as digital scanning to help identify early changes. That’s useful when the goal is to distinguish between a stain, an inactive area, and a lesion that still needs treatment.
For many patients, this is the moment the anxiety drops. Instead of wondering whether they need a filling, Invisalign, cosmetic dentistry, or more involved restorative dentistry, they finally know what the tooth needs.
A good exam should leave you with a clear answer, not more uncertainty.
If the area is early and non-cavitated, the plan may focus on monitoring, fluoride support, home care changes, or a minimally invasive treatment. If the tooth already has a true cavity, the discussion shifts to repairing it before it deepens.
Patients with anxiety often feel relieved to hear there may be gentle options available, including sedation dentistry when appropriate. And if the concern turns out not to be a cavity at all, that’s useful information too. Peace of mind is part of good care.
For anyone searching dentist in Fair Lawn, NJ, a thoughtful exam should feel practical, calm, and specific to your situation.
The best answer to can small cavities go away is a careful one. Early enamel damage may improve. A true cavity will not. The hard part is that these two stages can look very similar at home.
That’s why waiting and guessing rarely helps. If the spot is still reversible, early care gives you the best chance to protect the tooth conservatively. If the tooth already has a cavity, catching it now may help you avoid a more involved repair later. Either way, you gain clarity.
If you’ve been putting off an exam because the tooth only bothers you sometimes, or because you’re hoping better brushing will solve it, this is a good time to act. The earlier a dentist evaluates the area, the more options you usually have. That applies whether you need a simple check, cleaning and exams, a filling, an emergency visit, or a broader plan that may eventually include teeth whitening, dental implants near me, or other smile-focused treatment.
For families in Fair Lawn, Ridgewood, and Glen Rock, a timely exam can protect comfort, appearance, and long-term oral health. The goal isn’t to over-treat a small spot. It’s to understand it before it has a chance to become a bigger problem.
If you’ve noticed a white spot, dark groove, sensitivity, or a possible cavity, Dental Professionals of Fair Lawn can help you get a clear diagnosis and a personalized treatment plan. Schedule a consultation to protect your smile with compassionate care in Fair Lawn, NJ.