Traditional Fixed Bridge Guide for Fair Lawn, NJ Patients
Considering a traditional fixed bridge? Our Fair Lawn dentists explain the procedure, costs, and pros vs. cons compared to dental implants. Schedule a consult.
Considering a traditional fixed bridge? Our Fair Lawn dentists explain the procedure, costs, and pros vs. cons compared to dental implants. Schedule a consult.
A missing tooth has a way of showing up at the worst times. You notice it when you smile in a photo, when food keeps catching in the space, or when chewing on one side starts to feel awkward. For some people, the bigger issue is appearance. For others, it’s comfort, speech, or the worry that the neighboring teeth may start shifting.
If you’ve been searching for a dentist near me or a cosmetic dentist in Fair Lawn, you’re probably not looking for theory. You want to know what your options are, what the process feels like, and whether a traditional fixed bridge is the right choice for your smile.
A traditional fixed bridge is one of the classic ways to replace a missing tooth or several consecutive missing teeth. It’s called a bridge because it spans the gap. The replacement tooth sits in the open space, and the teeth beside that space help support it. For many patients in Fair Lawn, Ridgewood, and Glen Rock, it’s a practical, time-tested form of restorative dentistry that can restore function and help a smile look complete again.
When a tooth is missing, daily life changes in small ways first. You may chew more carefully. You may smile with your lips closed. You may even avoid certain foods because biting down doesn’t feel balanced anymore.
That’s where a traditional fixed bridge can make sense. It replaces the missing tooth with a restoration that stays in place, so you don’t remove it at night or take it out to clean it. Many patients like that it feels more like having teeth again, rather than wearing an appliance.
A bridge isn’t just about filling an empty space. It can help restore the shape of your smile and make chewing feel more natural. It can also support the overall harmony of your bite when it’s carefully planned.
At a consultation in Fair Lawn, the conversation usually starts with simple questions:
Those questions matter because the right solution depends on the condition of the surrounding teeth, your gum health, your bite, and your goals.
A good dental decision doesn’t start with the treatment. It starts with understanding what your mouth needs and what trade-offs come with each option.
For someone who wants a non-removable solution and may not be ready for implant treatment, a traditional fixed bridge can be a very reasonable option. It has been used for many years, and when planned well, it can look natural and function well.
Patients often ask some version of the same thing: “Will it look natural, and will I be able to eat normally?” Those are fair questions.
A well-made bridge is designed to blend with the surrounding teeth in shape and color. It’s also designed to help you chew with more confidence than you can with an unfilled gap. If you’re looking for a dentist in Fair Lawn, NJ who can walk you through restorative choices without pressure, that conversation should feel clear and honest from the start.
A traditional fixed bridge has three basic parts. The replacement tooth in the middle is called a pontic. The natural teeth on either side that support the bridge are called abutment teeth. Crowns fit over those abutment teeth, and the whole restoration is cemented into place as one connected piece.
That sounds technical, but the everyday version is simple. If there’s a gap where a tooth used to be, the bridge uses the neighboring teeth as supports so the new tooth can sit securely in the middle.

Think about a small bridge over a stream. The span in the middle only works if the structures on both sides are strong enough to hold it. Dentistry uses the same logic.
With a traditional fixed bridge, the middle tooth doesn’t stand on its own. The supporting teeth do the work of helping carry bite pressure. That’s why the health and strength of those supporting teeth matter so much.
Dentists use a design principle called Ante’s Law when planning many fixed bridges. In plain language, it means the combined root surface area of the supporting teeth should equal or exceed that of the tooth being replaced. This helps distribute forces in a way that lowers the risk of overload and failure. The same reference notes that following this principle is associated with 90% to 95% 10-year survival rates for fixed bridges in clinical literature (Ante’s Law and fixed bridge design principles).
That’s one reason bridge planning shouldn’t be rushed. It isn’t just about making something that looks good. It has to handle chewing pressure in a predictable way.
For many patients, the process is straightforward:
Evaluation
The dentist checks the missing area, the neighboring teeth, the gums, and the bite.
Preparation of the support teeth
The abutment teeth are shaped so crowns can fit over them.
Impressions or digital scans
These are used to design a custom bridge that fits your mouth.
Temporary restoration
A temporary bridge may protect the prepared teeth while the final one is made.
Final placement
The finished bridge is tried in, adjusted if needed, and cemented in place.
A fixed bridge stays in your mouth. You don’t take it in and out. That’s different from a removable partial denture, which comes out for cleaning and storage.
For many people, that fixed feel is a major reason to choose it. It can offer a sense of stability and familiarity that feels closer to natural teeth, especially when the bridge is well designed and the bite is balanced carefully.
A lot of dental anxiety comes from not knowing what will happen. Once patients understand the visit flow, the treatment usually feels much more manageable.
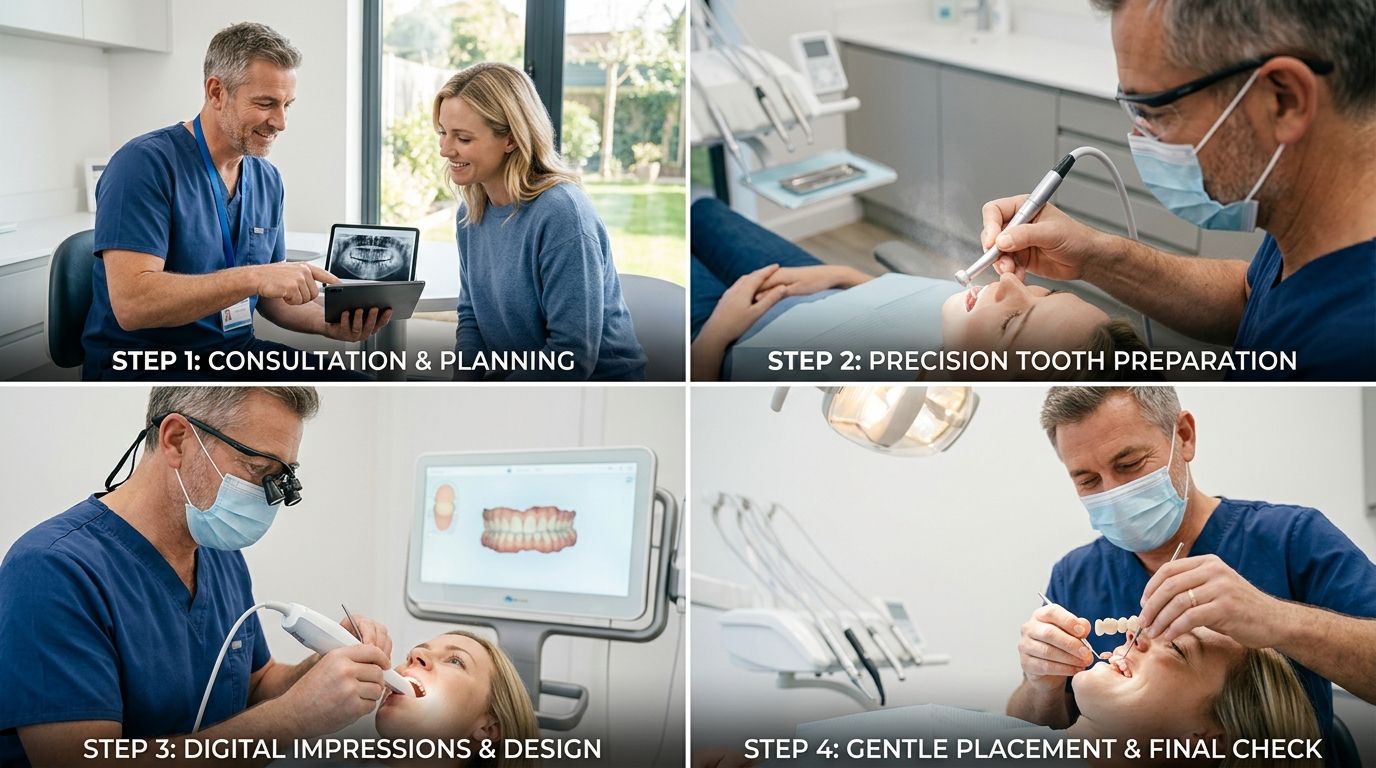
The first appointment starts with evaluation and planning. If you’re a new patient, that may include a full exam, dental x-rays, and a close look at the teeth next to the gap. The dentist also checks your gums, bite pattern, and whether the support teeth are good candidates for crowns.
If a bridge is appropriate, the abutment teeth are prepared. That means they’re reshaped so the final crowns can fit properly. A bridge needs enough space for durable materials and a natural contour, so this step is precise.
Many patients worry that this part will be uncomfortable. In reality, the visit is usually done with local anesthesia so the area is numb. If you’re nervous, sedation dentistry may also be discussed to help you feel more relaxed during treatment.
After the teeth are prepared, the next step is capturing the shape of your mouth. Modern offices often use digital scanning rather than traditional putty impressions. That improves precision and makes the process easier for patients with a strong gag reflex.
A temporary bridge is commonly placed before you leave. It helps protect the prepared teeth and keeps the space looking presentable while the custom bridge is being made.
A page on dental bridges in Fair Lawn can help you review the basic treatment option before or after your consultation.
Practical rule: The temporary matters. It protects the prepared teeth, helps you function between visits, and gives useful feedback about shape and comfort before the final bridge is cemented.
At the second appointment, the temporary is removed. The final bridge is checked for fit, appearance, and bite. This step matters more than many patients realize.
A bridge can look beautiful and still feel wrong if the bite is too high or the contacts aren’t balanced well. The dentist checks how the bridge meets the opposing teeth and makes small refinements before it’s permanently cemented.
Once everything looks and feels right, the bridge is bonded into place.
Here’s a short visual overview of how bridge treatment works in practice:
The prospect of a clear finish line is appealing. A traditional fixed bridge is often completed in fewer visits than implant-based treatment, which can make it attractive if you want to restore your smile without a surgical phase.
That said, there’s an important trade-off. The supporting teeth usually need to be permanently altered to hold the bridge. That’s why the decision isn’t just about speed. It’s about whether those neighboring teeth are already restored, whether they’re strong enough, and whether preserving untouched tooth structure should be a higher priority.
A traditional fixed bridge works best when the situation around the missing tooth supports it. The answer isn’t only “Do you have a gap?” The better question is “Do you have the right support for a bridge to last well?”
You may be a good candidate if:
A bridge can be especially reasonable when the adjacent teeth already need crowns. In that situation, preparing them for a bridge may fit the treatment plan more naturally.
Traditional bridges remain common, but they do ask something important of the neighboring teeth. The healthy natural teeth used to anchor them experience about a 30% failure rate within five to seven years following placement, primarily because of the structural changes required during preparation (traditional bridge anchor tooth failure consideration).
That doesn’t mean a bridge is a bad choice. It means the decision should be made with open eyes. If the adjacent teeth are already heavily filled, cracked, or in need of crowns, the trade-off may feel different than it would if those teeth are untouched and healthy.
| Feature | Traditional Fixed Bridge | Dental Implant | Removable Partial Denture |
|---|---|---|---|
| Support | Adjacent natural teeth | Jawbone through implant support | Clasps or framework around existing teeth |
| Impact on nearby teeth | Requires preparation of support teeth | Usually doesn’t rely on adjacent teeth | May place pressure on nearby teeth |
| Removability | Fixed in place | Fixed in place | Removed daily |
| Treatment feel | Faster path for many patients | More involved process | Least invasive approach |
| Best fit | When support teeth are suitable | When preserving neighboring teeth is a priority | When a removable option is preferred |
The right candidate for a bridge isn’t the person who wants the fastest option. It’s the person whose teeth, gums, bite, and goals line up with what a bridge needs to succeed.
Patients often walk into a consultation thinking they’re choosing between “bridge or implant.” In reality, there are usually three practical categories to discuss: a traditional fixed bridge, a dental implant, or a removable partial denture.
Each one solves the same problem in a different way.
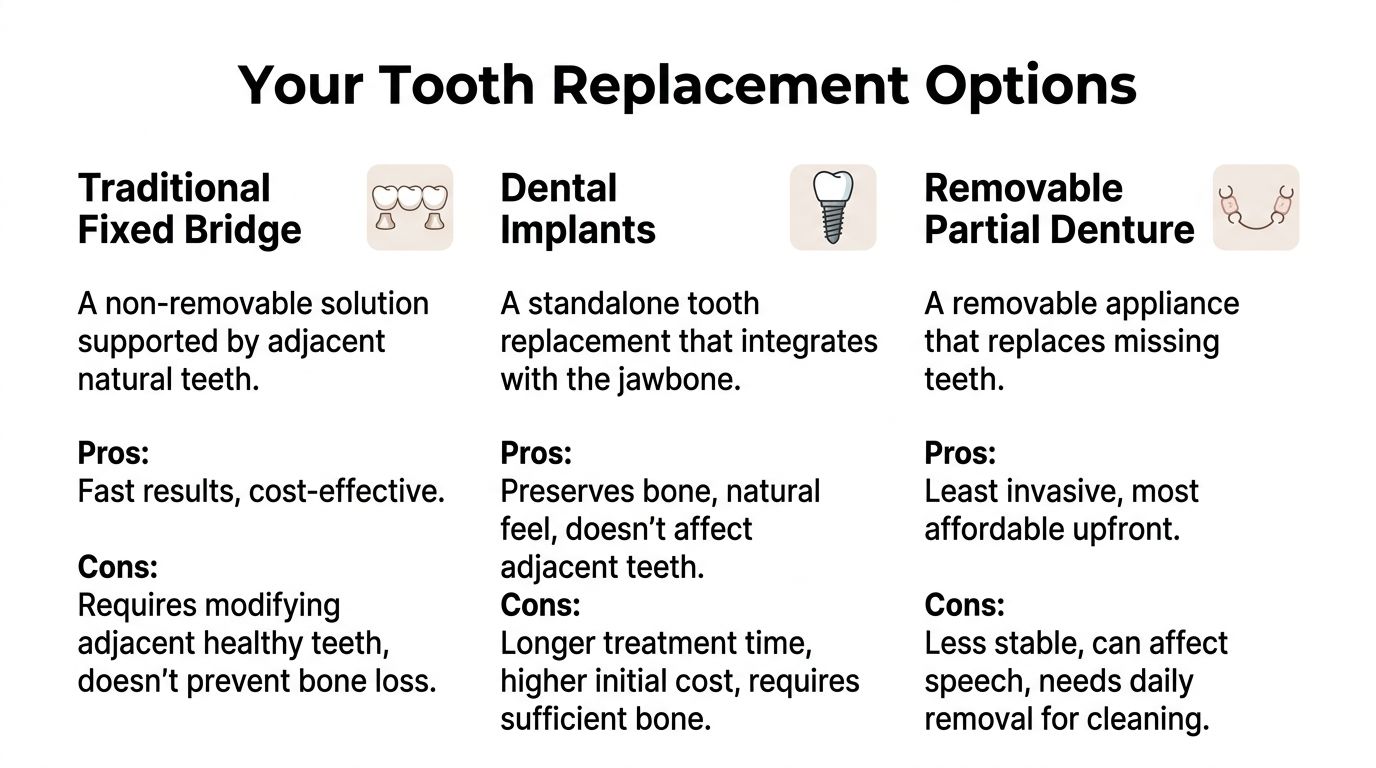
| Feature | Traditional Fixed Bridge | Dental Implant | Removable Partial Denture |
|---|---|---|---|
| How it stays in place | Supported by crowns on neighboring teeth | Supported by an implant placed in bone | Rests on gums and uses a removable framework |
| Surgery required | No | Yes | No |
| Effect on adjacent teeth | Requires reshaping support teeth | Usually preserves adjacent teeth | May affect comfort around nearby teeth |
| Cleaning | Needs careful cleaning under the pontic | Brushed and flossed like a single restoration, depending on design | Removed for cleaning |
| Timeline | Often shorter than implant treatment | Longer overall process | Often simpler to deliver |
| Feel in the mouth | Fixed | Fixed | Removable |
| Best use case | Missing tooth with suitable support teeth | Missing tooth with healthy neighboring teeth and implant candidacy | Patients seeking a removable option |
For patients comparing choices in more detail, this guide on dental implants vs bridges and which option is right for you is a useful follow-up.
A traditional fixed bridge can make sense when:
The neighboring teeth already need crowns
If those teeth are already damaged or restored, using them as bridge supports may fit naturally into the treatment plan.
You want to avoid surgery
Some patients prefer a non-surgical option because of medical history, personal comfort, or timing.
You want a fixed result in a shorter treatment window
A bridge often reaches the finish line faster than implant treatment.
An implant may be favored when:
The teeth beside the gap are healthy and untouched
Preserving those teeth can be a major advantage.
The missing span is long
Span length matters. Clinical research on tooth-supported fixed dental prostheses found 28% complication rates for long-span bridges over 5 years, compared with 12% for short-span bridges over the same period (bridge span length and complication rates).
You want support that doesn’t depend on adjacent crowns
That can simplify force distribution and reduce the burden on neighboring teeth.
Partial dentures still have a place. They can be helpful for patients who want a less invasive route or need a solution that doesn’t require crown preparation or implant surgery.
They do come with compromises. Because they’re removable, some patients notice more movement, more awareness in the mouth, and a different chewing feel than they’d get from a fixed solution.
No single option wins for everyone.
A bridge may be practical and efficient. An implant may be more conservative toward neighboring teeth. A partial denture may be the most realistic path for some situations. Good treatment planning means matching the option to the person, not forcing the person into the option.
A traditional fixed bridge has stayed relevant for a reason. It can solve a visible and functional problem without surgery, and it can do so with a result that looks very natural when designed well.
Still, it’s one of those treatments that deserves a balanced explanation. Patients make better decisions when they understand both what a bridge does well and where caution is needed.
A fixed bridge offers several practical advantages:
No surgical phase
For patients who don’t want implant surgery, this is often the first reason they consider a bridge.
A shorter path to replacing the tooth
Treatment is usually more direct than an implant process.
A stable, non-removable restoration
Many people prefer something that stays in place rather than a removable appliance.
Natural appearance
The bridge can be shaped and shaded to blend with the surrounding smile.
The main drawback is that the supporting teeth are part of the treatment. They must be prepared for crowns, and that creates long-term responsibility for those teeth.
A systematic review reported that abutment teeth have a 12% to 18% failure rate within 10 years, with failures driven mainly by secondary decay and periodontal issues (abutment teeth long-term risk in bridge treatment).
That statistic matters because it changes how a bridge should be maintained. The bridge itself may look fine from the outside while problems begin around the margins of the supporting crowns or in the surrounding gum tissue.
Bridge maintenance needs to be deliberate, especially around the support teeth.
Brush carefully along the gumline
Plaque at the crown margins can lead to trouble over time.
Clean under the pontic every day
A floss threader or water flosser can help reach the area beneath the replacement tooth.
Keep routine cleanings and exams on schedule
Professional checks help catch margin problems early.
Don’t ignore small symptoms
A new odor, trapped food, gum bleeding, or a change in bite should be evaluated.
If you choose a bridge, the most important habit isn’t just brushing the visible surfaces. It’s cleaning the hidden areas where problems usually start.
A traditional fixed bridge can be an excellent restoration when the case selection is sound and the patient is committed to upkeep. It’s not “good” or “bad” in the abstract. It’s appropriate in some mouths and less ideal in others.
Once a bridge is in place, the daily goal is simple. Keep the bridge clean, protect the supporting teeth, and make it easy for your dentist to monitor the area over time.
With proper care, traditional fixed bridges have shown strong longevity. Clinical studies have reported that 74% of bridges remain durable after 15 years, and other analyses found survival rates as high as 97% past the 5-year mark (long-term bridge durability and survival data).
Most bridge problems don’t start with a dramatic event. They start subtly, with plaque building around the edges or under the pontic.
A practical routine usually includes:
Brush twice daily
Focus on the gumline around the crowned support teeth.
Use a floss threader or bridge floss
This helps clean beneath the replacement tooth where standard floss can’t pass straight through.
Consider a water flosser
Many patients find it easier to clean under a bridge consistently with water irrigation.
Clean after sticky or fibrous foods
Foods that pack into the bridge area can sit there longer than you think.
You don’t need to be fearful about eating, but smart habits help.
Try to be careful with very sticky candies, chewing ice, or using your teeth to open packaging. A bridge is strong, but it isn’t indestructible. Repeated stress or poor hygiene is what usually shortens the life of restorations.
Small changes matter with bridges. Call for an exam if you notice:
A bridge often lasts longest when problems are handled early, before they turn into decay under a crown or damage to a support tooth.
Regular cleanings and exams aren’t just routine maintenance. They give your dentist a chance to check the margins of the crowns, the health of the gums, and how the bridge is handling bite forces over time.
For many patients, that’s the difference between a bridge that serves well for years and one that develops hidden complications. Daily care at home does the heavy lifting. Professional monitoring helps protect the result.
Choosing a bridge usually brings up a second round of practical questions after the first consultation. Patients want to know if it will hurt, what they’ll be able to eat, whether insurance may help, and how to balance a bridge against alternatives like implants or dentures.
The good news is that those questions can usually be answered clearly once your exam is complete and the condition of the surrounding teeth is known.
Will the procedure hurt?
Most patients do well with local anesthesia during tooth preparation. If you tend to feel anxious in the dental chair, ask about sedation options.
What can I eat after placement?
Right after treatment, softer foods are often easier while you adjust. Once the bridge feels settled and your bite feels natural, most patients return to a normal diet with sensible care.
Will insurance cover a bridge?
Coverage depends on your plan, waiting periods, and frequency limitations. A front desk team can usually help review benefits and explain what’s known before treatment begins.
How do I know whether a bridge or implant is better for me?
That depends on the health of the neighboring teeth, your gum and bone condition, your bite, your timeline, and whether you want to avoid surgery.
A bridge consultation should not feel rushed. You should leave understanding:
For patients who like to handle healthcare logistics more efficiently, tools that support smoother communication can help. If you’re curious how modern practices are using technology to reduce scheduling friction, this overview of AI for scheduling patient appointments offers useful context.

A thoughtful consultation is where confidence starts. You don’t need to walk in knowing the answer. You just need a clear evaluation, honest guidance, and a plan that fits your health and goals in Fair Lawn.
If you’re ready to replace a missing tooth and want a clear, pressure-free conversation about your options, schedule a consultation with Dental Professionals of Fair Lawn. A personalized exam can help you decide whether a traditional fixed bridge, dental implant, or another restorative solution makes the most sense for your smile.